What If You Have Private Insurance And Medicare
If you already have healthcare coverage through a commercial insurer when you become eligible for Medicare, you have the option to keep both types of insurance and the option to use both. Your private plan can be the primary payer that handles your healthcare costs before Medicare does, or the private plan can be secondary to Medicare. Your choice depends on individual circumstances. One critical consideration: Medicare requires everyone 65 and older to have adequate prescription drug coverage defined as and your employer plan may not qualify.
You may choose to build your primary health coverage on private insurance if your spouse relies on that plan for coverage, or choose Medicare as your primary insurer after considering the deductibles, copayments, and coinsurances of both options.
Medicare and other insurance plans coordinate to avoid duplicate payments. If Medicare is your primary payer, it will pay first and then your private plan will kick in to cover some or all of the remaining costs. If Medicare is secondary, then the opposite occurs. Typically, Medicare cannot be changed from a primary payer to a secondary payer.
Whether Medicare is primary or secondary to existing insurance generally depends on the source of the other insurance policy. If you are uncertain about which insurer is your primary or secondary, you can check with your private plan or call Medicares Benefits Coordination & Recovery Center at 1-855-798-2627.
Who Qualifies For Medicare Parts A And B
Your become eligible for Medicare in one of three ways:
-
When you reach age 65
-
If you have a disability
-
You become disabled with permanent kidney failure or amyotrophic lateral sclerosis
Medicare is divided into several different parts: Part A covers costs related to hospitalization, while Part B covers expenses related to visits to your healthcare providers as well as any other care you receive as an outpatient.
Another Coverage Choice If You Have Esrd
You might be eligible for a Special Needs Plan, a specific type of Medicare Advantage plan that targets individuals who live in an institution, have Medicaid, or have certain chronic conditions . These plans include prescription drug coverage as part of the plan, and a Chronic-Condition Special Needs Plan for people with ESRD may also cover certain services to help you manage your condition. If there is a Special Needs Plan for beneficiaries with end-stage renal disease in your area, you may be able to enroll and get your Medicare benefits that way.
Read Also: Can Chocolate Cause Kidney Stones
What Supplies Do You Need For Home Dialysis
There are different kinds of home dialysis, and each uses different equipment to remove toxins from your bloodstream. While there are differences between the machines and how they operate, all Medicare beneficiaries who need at-home dialysis can expect Medicare to cover some standard supplies, including:
- Dialysis machine
- Sterile drapes
Outpatient Maintenance Dialysis Treatments

Routine dialysis, ESRD-related lab tests and other outpatient care is typically covered by Medicare Part B if you get these services at a Medicare-certified dialysis facility.
- How much does Medicare pay for outpatient dialysis treatment?Once you pay your Part B deductible, you pay 20 percent of the Medicare-approved amount for each dialysis treatment given in a dialysis facility or at home.
Recommended Reading: Red Wine Kidney Stones
Can You Appeal A Denial Of Coverage For Home Dialysis Equipment Or Services
Sometimes, Medicare may deny coverage for a service or equipment related to your home dialysis. An appeal is the action you can take if you disagree with the decision. For example, you can file an appeal if Medicare or your Medicare Advantage plan:
-
Denies a request for a service, supply, item, or prescription drug that you think should be covered by your plan
-
Denies a request for payment of a healthcare service, supply, item, or prescription drug you already have received
-
Denies a request to change the amount you are required to pay for a healthcare service, supply, item, or prescription drug
-
Has stopped providing or paying for all or part of a healthcare service, supply, item, or prescription drug you believe you still need
Appeals tend to be the most successful when your doctor is supportive by deeming the service, supply, item, or prescription drug medically necessary or if you have reason to believe that there was a processing error that led to your coverage denial. Medicare has issued an official booklet that explains the appeals process in detail.
How To Qualify For Medicare
Besides needing dialysis or a kidney transplant, to get Medicare for kidney failure, you need to have work credits. You earn credits by earning money in each quarter of a year. Each year, the amount you must earn to gain a credit goes up. In 2007, you need to earn at least $1,000 in a quarter to earn a credit. You can earn up to 4 credits a year.
The younger you are, the fewer work credits you need. If you’re under 24, the most credits you would need is 6. If you’re 24 through 30, you need more. By age 62, you need 40 credits. Social Security can tell you how many credits you have and how many you need.1
Haven’t worked outside the home? You may still qualify for Medicare if your spouse has worked enough. Even if you’re divorced or widowed, a former spouse’s credits count for your Medicare if you were married for at least 10 yearsand haven’t remarried before age 60.
A parent’s work credits can qualify a child for Medicare, too. And, in some cases, an adult child’s work credits can help a dependent parent over age 65 to qualify.
Recommended Reading: How Do You Know If You Have Bad Kidneys
What Other State Programs Can Help
Medicare Savings Programs are programs in which your state may pay your Medicare premiums, deductibles, and/or coinsurance if you have a low income and few assets. How Medicaid works in U.S. territories varies. Learn more about how your state Medicaid works online.
State Health Insurance Assistance Programs give local advice about health insurance to people who have Medicare or who are eligible for Medicare. SHIP counselors can help you choose the best plan for your needs. Find a SHIP counselor at shiptacenter.org or call 1-877-839-2675.
State kidney programs provide financial help and other services to people with kidney disease. Talk with your dialysis or transplant clinic social worker or financial counselor to find out if your state has a kidney program.
State Pharmaceutical Assistance Programs help pay for prescription medicines in certain states. Learn whats available in your state with the SPAP online locator.
Immunosuppressant Drugs For Dialysis
Youll need immunosuppressant drugs for life when you get a kidney transplant. While this sounds scary and costly, you can take a breath of relief.
Part B will cover these drugs under a few different factors:
- Part A benefits covered your transplant.
- You have Part B coverage when its time to fill the prescription.
- Youre eligible for Medicare ESRD.
Part B wouldnt cover immunosuppressants if you didnt have Part A during your surgery. If this situation applies to you, you may need to buy a Part D plan to cover the medications you need.
Recommended Reading: Constipation Kidney Stones
Medicare Advantage Plans Esrd And Dialysis Coverage
Generally, you cannot enroll in a Medicare Advantage plan if you have already been diagnosed with end-stage renal disease. But there are two prominent exceptions.
Exceptions for Medicare Advantage Coverage of ESRD
- If you have insurance through your job provided by the same company that offers a Medicare Advantage Plan, you can enroll in that companys Medicare Advantage plan.
- You can enroll in a Medicare Advantage Special Needs Plan if it specifically serves people who have end-stage renal disease.
However, if you enrolled in a Medicare Advantage plan before you developed ESRD, you cannot be kicked off the plan. And if the plan leaves Medicare or leaves your service area, you will have a special enrollment period to sign up for another Medicare Advantage plan where you live.
I Have Private Insurance Through The Affordable Care Act
- You do not need to apply for Medicare at any time unless you choose to. If you choose to apply for Medicare, and your private insurance plan is through the Affordable Care Act, you will lose your private plan coverage. This is because Affordable Care Act insurance plans are for people who no other insurance options. Once you have Medicare, you are considered to have other coverage and would no longer qualify for coverage through the Affordable Care Act.
Recommended Reading: Can Grape Juice Change Urine Color
What Is The Cost Of Dialysis With Medicare
The average cost of dialysis treatments is approximately $500 per treatment for individuals without insurance. Medicare recipients are generally required to pay a deductible of approximately $150 and a 20% coinsurance cost. Medicare covers the remaining 80%. Recipients who are part of a Medigap Supplemental plan may qualify for partial or full coverage of the required 20% coinsurance payment.
When Medicare Coverage Ends For Esrd
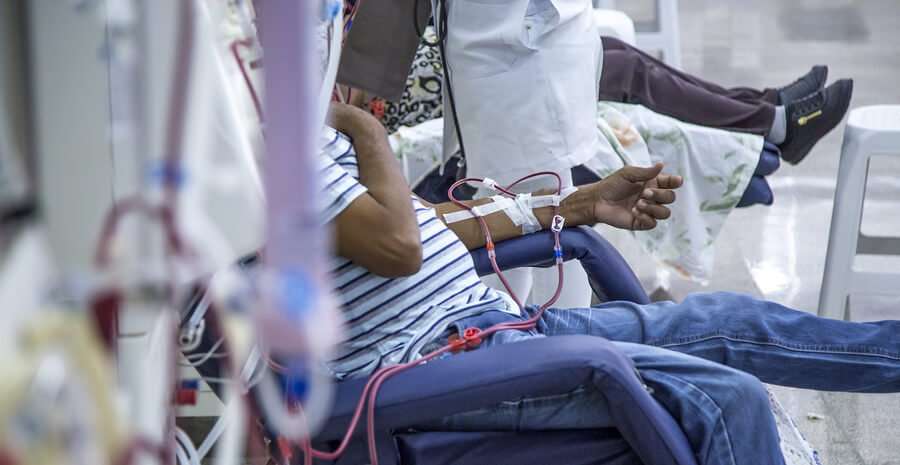
If a Medicare patient only has Medicare because of permanent kidney failure, Medicare coverage will end:
-
12 months following the cessation of dialysis treatment
-
36 months after a kidney transplant
However, coverage can resume again in certain situations. Visit Medicares official website to learn more.
Don’t Miss: Ginger Good For Kidney
Medicare Advantage Dialysis Coverage
As of January 2021, people with ESRD can join a Medicare Advantage planMedicare Advantage , also known as Medicare Part C, are health plans from private insurance companies that are available to people eligible for Original Medicare ….. Previously, only Original MedicareOriginal Medicare is private fee-for-service health insurance for people on Medicare. It has two parts. Part A is hospital coverage. Part B is medical coverage…. was available to people diagnosed with ESRD. Special Needs Plans may be available in some areas to address the specific needs of ESRD patients. SNP-C plans are customized to the particular needs of their covered condition, providing benefits and additional services that go beyond what Medicare usually covers, which can include:Medicare.gov, I have End-Stage Renal Disease , Accessed November 24, 2021
- A care team of specialists for the special condition
- A case coordinator to optimize the coordination of services you need
- Extra hospital days
- Drug coverage formularies tailored to your condition
These benefits may not be available for every Medicare Advantage SNP. Ask your local Medicare Advantage providers about which SNPs they offer and what benefits they provide.Medicare.gov, I have End-Stage Renal Disease , Accessed November 24, 2021
How Do You Apply For Medicare Parts A And B
Youre first eligible to sign up for Medicare 3 months before you turn age 65 or earlier, if you have a disability, ESRD, or ALS. After you turn 65, you can sign up for Medicare Part A with or without Part B. You have a 7-month window for Medicare Part A enrollment that begins 3 months before you turn 65, includes your birth month, and ends 3 months after you turn 65.
If you already receive Social Security retirement or disability benefits at the time you turn 65, you are usually automatically enrolled in Medicare Part A and Part B.
The fall open enrollment is the time period when Medicare beneficiaries and those enrolling can make the most changes to their coverage. Its open to everyone eligible for Medicare every year from . You can enroll in Medicare by visiting its website and following the instructions.
Don’t Miss: Is Watermelon Good For Kidney
How Do I Enroll In A Medicare Advantage Plan
There are many ways to join Medicare Advantage plans, including:
- Visit the State Health Insurance Assistance Program at SHIPHelp.org
- Talk to an independent licensed insurance agentlike one from SelectQuote. SelectQuote can help you understand your insurance options and compare health insurance plans available to you. To contact SelectQuote, call 1-877-213-1342 or visit SelectQuote.com/FreseniusKidneyCare.
Medicare And Chronic Kidney Disease
Medicare is a federally funded health insurance program for Americans over age 65 and people who have been deemed disabled. In 1972, people requiring dialysis became newly entitled to this health benefit. The law was amended in order to provide coverage to people who may have forgone treatment due to the high costs of dialysis treatment. Today, if you have chronic kidney disease and need dialysis, you may be eligible for Medicare insurance.
Medicare is health insurance for people who fit one of the following 3 categories:
- Age 65 or older
- ESRD any age person with end stage renal disease
Medicare has the following parts:
- Part A Covers all inpatient services
- Part B Covers all clinical outpatient services
- Part C Such as HMO or PPO
- Part D Offered to anyone with Medicare
Medicare drug plans are run by insurance companies and other private companies approved by Medicare.
Age If you get benefits from Social Security or the Railroad Retirement Board, you are automatically entitled to Medicare Part A and Part B starting the first day of the month you turn age 65.Your Medicare card will be mailed to you about 3 months before you turn 65. However if youre still actively working you may not be required to obtain Medicare due to age.
Patients with ESRD who begin home dialysis have an additional advantage regarding Medicare coverage. If you choose a home dialysis therapy you can qualify for Medicare immediately upon the initiation of dialysis.
Table 1.
Summary
Don’t Miss: Is Apple Cider Vinegar Good For Kidneys
When Medicare Coverage Starts For Esrd
Eligibility for Medicare coverage due to ESRD is different from other types of Medicare eligibility. If someone is eligible for Medicare because of ESRD and doesnt enroll immediately, their coverage could still begin up to 12 months prior to the month they apply, known as retroactive coverage. How this looks will depend on whether they are on, or need, dialysis, or require a kidney transplant.
In the event a Medicare patient is on dialysis, their coverage typically begins on the first day of the fourth month of dialysis treatment. Do note, this four-month waiting period starts even if someone hasnt yet signed up for Medicare.
If someone is covered by an employer group health plan, their coverage will still begin the fourth month of dialysis. As well, the group health plan may cover the first three months of treatment.
Medicare coverage begins as soon as the first month of a regular course of dialysis treatments if all of the following are true:
-
The patient participates in a home dialysis training program during the first three months of a regular course of dialysis
-
The patients doctor expects them to complete home dialysis training, meaning they can perform self dialysis at home
-
They continue regular course dialysis treatments throughout the waiting period
Medicare coverage for kidney transplants works differently than dialysis. Learn more at this resource. Learn more at this resource.
How Does Medicare Cover Dialysis
Medicare covers most supplies and services needed for dialysis, including:Medicare.gov, Dialysis services & supplies, Accessed November 24, 2021
- Inpatient dialysis treatments
- Most drugs for in-facility and at-home dialysis
- Other services and supplies, such as laboratory tests
- Dialysis when you travel in the U.S. and its territories
If youre under the age of 65 and have End-Stage Renal Disease , you may qualify for enrollment in Medicare without meeting the normal age limit. Medicare coverage obtained this way is not limited only to ESRD services and treatments. You can use Medicare for all the services that it normally covers.Medicare.gov, I have End-Stage Renal Disease , Accessed November 24, 2021
Read Also: Is Almond Milk Bad For Kidney Stones
When Will My Esrd
If you qualify for Medicare benefits based on ESRD and youre currently on dialysis, your Medicare coverage typically starts the first day of your fourth month of dialysis treatment. Coverage can begin on the first month of treatment if:Medicare.gov, I have End-Stage Renal Disease , Accessed November 24, 2021
If youre admitted for a kidney transplant and the transplant takes place within two months, Medicare benefits will begin the month you are admitted. Medicare coverage can begin two months prior to your transplant if the transplant is delayed more than two months.Medicare.gov, I have End-Stage Renal Disease , Accessed November 24, 2021
What Is Included In A Dialysis Bundle
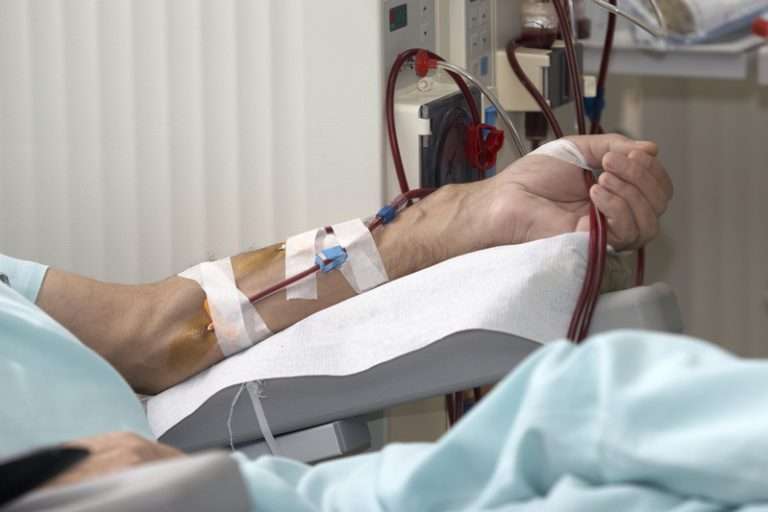
The dialysis bundle, technically referred to as the Medicare ESRD Bundle, is a bundled payment for the costs of dialysis, labs, supplies and medications. Medicare Part B pays for all bundled items in a single payment instead of making multiple separate payments for each individual service. Recipients are required to pay 20% coinsurance responsibility, and Medicare continues to pay 80% of the costs.
Also Check: Red Wine And Kidney Stones
What Is Kidney Disease
Kidney disease happens gradually as the kidneys lose their ability to filter out liquid waste effectively. Over time, these liquids can build up in your body, causing a range of dangerous symptoms. Kidney disease usually happens as the result of another health problem, such as diabetes or high blood pressure. It can also occur due to ongoing kidney infections or cysts and inflammation in the kidneys.
When kidney disease starts, you may not have many symptoms, making it very difficult to catch and treat. Kidney disease symptoms can include nausea and vomiting, fatigue, loss of appetite, changes in urination patterns, swelling of the lower extremities, and shortness of breath. Over time, kidney disease can cause serious cardiovascular complications, and it can also cause dangerous levels of fluid retention.