Medication To Protect Your Kidneys
- ACE inhibitors and ARBs. If you have high levels of protein in your urine then you may be advised to take medication even if your blood pressure is normal. Two related types of medication have been shown to be beneficial for many people with CKD. This is because they can prevent further worsening of the function of your kidneys. These medicines are called:
- Angiotensin-converting enzyme inhibitors and
- Angiotensin receptor blockers , such as losartan, valsartan, candesartan, telmisartan).
- SGLT2 inhibitors. A group of medicines called the SGLT2 inhibitors were originally used to keep blood sugar under control in type 2 diabetes. However, more recent studies show that some of them can significantly reduce decline in kidney function. These may be recommended whether you have type 2 diabetes or not. The National Institute for Health and Care Excellence has issued new guidance recommending that they should be offered to, or considered for, most people with type 2 diabetes and CKD.
Does Chronic Kidney Disease Cause Stomach Bloating
Kidney Problems Cause Stomach Bloating: A person with chronic kidney disease and/or diabetes should take precautions if they are facing stomach bloating because it could be a sign of severe complications. Along with that, this may provide you with bloating, pain on swallowing, sore throat, heartburn, fullness, nausea, vomiting, diarrhoea, and constipation.
Blood Tests For Kidney Disease
The best measure of kidney function is the glomerular filtration rate , which can be estimated from a blood test that checks the blood for creatinine .
A normal GFR result is higher than 90 mL/min/1.73 m2. If the result is persistently less than 60 mL/min/1.73 m2 for at least three months, this confirms that the person has chronic kidney disease.
Blood tests can reveal other abnormalities of kidney function, such as:
- high levels of acids
- anaemia
- high levels of potassium
- low levels of salt
- changes to the levels of calcium and phosphate.
Also Check: Wine And Kidney Stones
Diagnosis Of Chronic Kidney Disease
-
Blood and urine tests
-
Sometimes biopsy
Blood and urine tests are essential. They confirm the decline in kidney function.
When loss of kidney function reaches a certain level in chronic kidney disease, the levels of chemicals in the blood typically become abnormal.
-
Urea and creatinine, metabolic waste products that are normally filtered out by the kidneys, are increased.
-
Blood becomes moderately acidic.
-
Potassium in the blood is often normal or only slightly increased but can become dangerously high.
-
Calcium and calcitriol in the blood decrease.
-
Phosphate and parathyroid hormone levels increase.
-
Hemoglobin is usually lower .
Potassium can become dangerously high when kidney failure reaches an advanced stage or if people ingest large amounts of potassium or take a drug that prevents the kidneys from excreting the potassium.
Analysis of the urine may detect many abnormalities, including protein and abnormal cells.
Ultrasonography is often done to rule out obstruction and check the size of the kidneys. Small, scarred kidneys often indicate that loss of kidney function is chronic. Determining a precise cause becomes increasingly difficult as chronic kidney disease reaches an advanced stage.
Removing a sample of tissue from a kidney for examination may be the most accurate test, but it is not recommended if results of an ultrasound examination show that the kidneys are small and scarred.
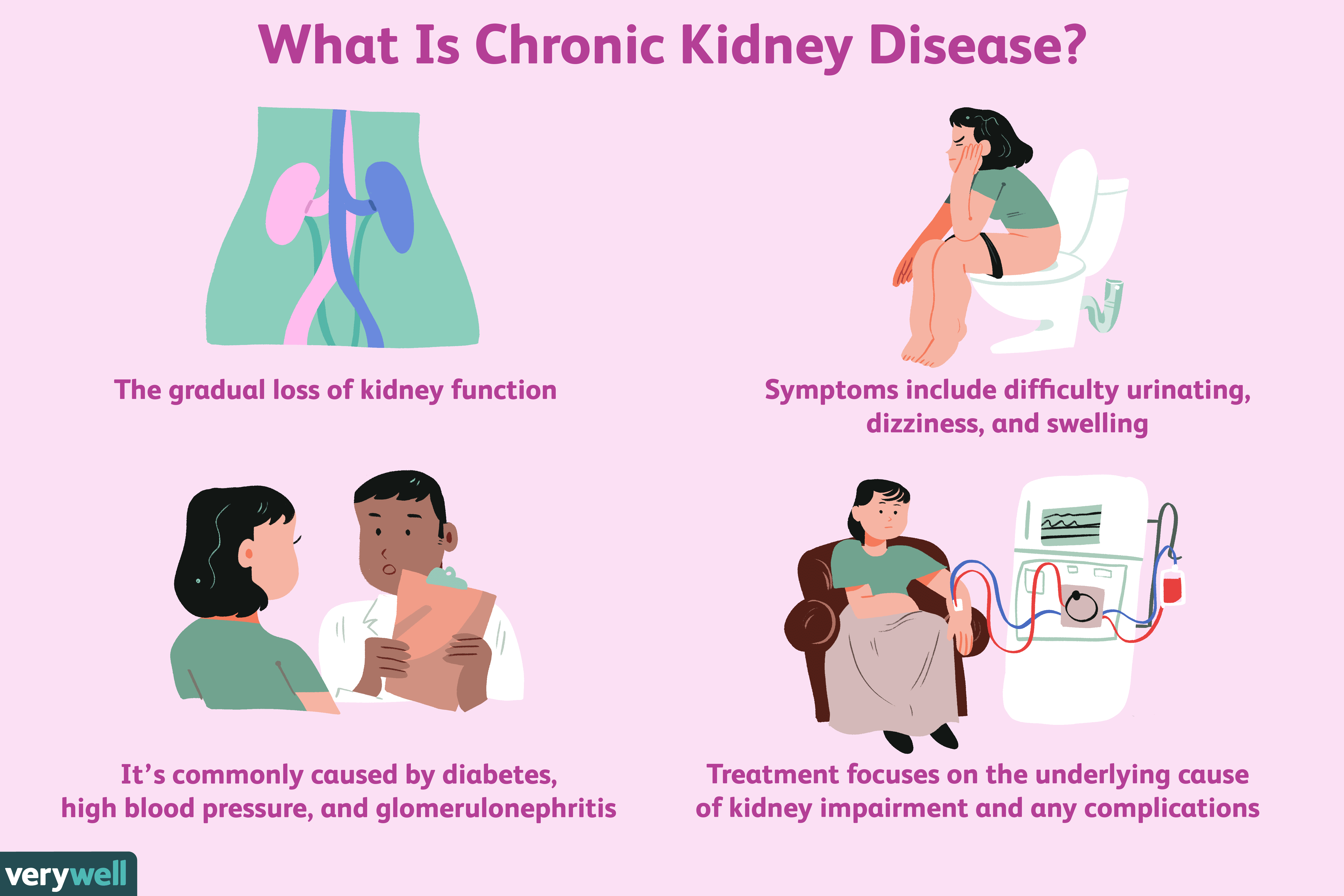
What Is Chronic Kidney Disease
Chronic kidney disease is long-term damage to the kidneys, the organs responsible for producing urine. Causes of chronic kidney disease include diabetes, hypertension, kidney infections, and inflammatory diseases, medications or toxins, inherited kidney diseases, and prematurity and low birth weight.
Symptoms include swelling and decreased urine output , fatigue, weakness, chest pain, shortness of breath, bone pain, nausea and vomiting, and neurological symptoms.
Diagnosis is made by laboratory tests. Chronic kidney disease is defined by laboratory evidence of kidney damage or decreased kidney function for three or more months.
Treatments include dietary changes and medications to treat the symptoms, slow progression of the disease, and manage complications. End-stage chronic kidney disease requires treatment with renal replacement therapy, which includes dialysis and kidney transplant.
You should make an appointment with your primary care physician to discuss your symptoms as soon as possible.
You May Like: How Do You Know If You Have Bad Kidneys
Signs Of Kidney Problems During Pregnancy
Preeclampsia
Preeclampsia affects only pregnant women after the 20th week of pregnancy and resolves shortly after the baby is delivered. Although it is by origin not a primary kidney problem, it does involve the kidneys. It is characterised by:
- Hypertension
- Proteinuria, or protein in the urine
Other symptoms which may appear as part of preeclampsia or as preeclampsia progresses include:
- Headache that cannot be alleviated with painkillers
- Edema of hands, arms, face and/or feet
- Blurred vision, other visual disturbances or blind spots
- Confusion or disorientation
- Oliguria of 500ml or less over 24 hours
- Being unable to feel the baby move as much as previously
- Shortness of breath, possibly due to pulmonary edema
- Stroke. This is very rare
Good to know: If a pregnant person suddenly discovers that their watch, bracelets or rings no longer fit their arm or hand, or that their sleeves are suddenly tight, they should seek medical help immediately. Preeclampsia can lead to eclampsia and HELLP Syndrome and is considered a medical emergency.
For more information on, see this resource on preeclampsia, eclampsia and HELLP Syndrome.
If you are concerned that you or a loved one may have preeclampsia, eclampsia or HELLP Syndrome, download the Ada app for a free symptom assessment.
Read Also: Is Cacao High In Oxalates
Warning Disclaimer Use For Publication
WARNING: Please DO NOT STOP MEDICATIONS without first consulting a physician since doing so could be hazardous to your health.
DISCLAIMER: All material available on eHealthMe.com is for informational purposes only, and is not a substitute for medical advice, diagnosis, or treatment provided by a qualified healthcare provider. All information is observation-only. Our phase IV clinical studies alone cannot establish cause-effect relationship. Different individuals may respond to medication in different ways. Every effort has been made to ensure that all information is accurate, up-to-date, and complete, but no guarantee is made to that effect. The use of the eHealthMe site and its content is at your own risk.
If you use this eHealthMe study on publication, please acknowledge it with a citation: study title, URL, accessed date.
Recommended Reading: Is Pomegranate Juice Good For Kidney Stones
Treating Pain In Patients With Chronic Kidney Disease: A Review Of The Literature
Patients with chronic kidney disease often suffer from chronic pain. It may be difficult to select appropriate analgesic therapy in this population because many patients require complex medication management for the comorbidities that accompany renal disease. A reduced glomerular filtration rate alters the normal pharmacokinetics of analgesic medications and increases the potential for toxicity, undesirable side effects, and drug interactions. Appropriate analgesic selection, dose titration, and monitoring are critical for the successful management of this population.
What Medications Are Prescribed For People With Chronic Kidney Disease
Depending on the cause of your kidney disease, you may be prescribed one or more medications. Medications your nephrologist may prescribe include:
- An angiotensin-converting enzyme inhibitor or an angiotensin receptor blocker to lower your blood pressure.
- A diuretic to help your body eliminate extra fluid.
- Medications to lower cholesterol levels.
- Erythropoetin, to build red blood cells if you are anemic.
- Vitamin D and calcitrol to prevent bone loss.
- Phosphate binder if your kidneys cant eliminate phosphate.
Also Check: Red Wine And Kidney Stones
Fatigue Being Tired All Of The Time
Why this happens:
Healthy kidneys make a hormone called erythropoietin , or EPO, that tells your body to make oxygen-carrying red blood cells. As the kidneys fail, they make less EPO. With fewer red blood cells to carry oxygen, your muscles and brain tire very quickly. This is anemia, and it can be treated.
What patients said:
I was constantly exhausted and didn’t have any pep or anything.
I would sleep a lot. I’d come home from work and get right in that bed.
What Is Good Kidney Disease Care
According to a national review, kidney disease services should:
- identify people at risk of kidney disease, especially people with high blood pressure or diabetes, and treat them as early as possible to maintain their kidney function
- give people access to investigative treatment and follow them up to reduce the risk of the disease getting worse
- give people good-quality information about managing their condition
- provide information about the development of the disease and treatment options
- provide access to a specialist renal team
- give people access to transplant or dialysis services if required
- provide supportive care
Your treatment for kidney disease will need to be reviewed regularly.
It may be helpful for you to make a care plan because this can help you manage your day-to-day health. Your kidney disease specialist nurse may be able to help with this.
You May Like: Tamsulosin Hcl 0.4 Mg Capsule For Kidney Stones
How Do I Get Help
Dr. Miller is a board-certified internist with extensive experience treating all types of internal pain. After a thorough review of your medical history, as well as testing, Dr. Miller will recommend the best treatment for your pain. If youve been experiencing pain in your upper back, and especially if youve been having other symptoms, at 813-336-3793 for an appointment.
You Might Also Enjoy…
- 4.89/5
Correction Of Phosphate Balance

If you have stage four or five kidney disease, you can get a build-up of phosphate in your body because your kidneys cannot get rid of it. Phosphate is a mineral that, with calcium, makes up most of your bones. Phosphate is obtained through diet, mainly dairy foods. The kidneys usually filter out excess phosphate. If phosphate levels rise too much, it can upset the normal calcium balance of the body. This can lead to thinning of the bones and furring of the arteries.
You may be asked to limit the amount of phosphate in your diet. Foods high in phosphate include red meat, dairy produce, eggs and fish. Your GP or dietitian should be able to advise you about how much phosphate you can eat. However, there is no advantage in reducing your intake of these foods unless you have a raised phosphate level. Always ask a healthcare professional before changing your diet.
If reducing the amount of phosphate in your diet does not lower your phosphate level enough, you may be given medicines called phosphate binders. These medicines bind to the phosphate in the food inside your stomach and stop it from being absorbed into your body.
To work properly, phosphate binders must be taken just before meals. The most commonly used phosphate binder is calcium carbonate, but there are also alternatives that may be more suitable for you.
The side effects of phosphate binders are uncommon but include:
- nausea
- itchy skin
Recommended Reading: Does Seltzer Water Cause Kidney Stones
What Are The Complications Of Mineral And Bone Disorder
The complications of mineral and bone disorder include
- slowed bone growth and bone deformities
- bone fractures
- heart and blood vessel problems
People who experience these complications may have a poorer quality of life, may spend more time in the hospital, and have a higher risk of fractures or death.3
How Kidney Issues Can Cause Back Pain
Back pain affects an estimated 80% of people, with many people experiencing chronic pain throughout their lives. Whats more, the causes of back pain can be surprising.
Our compassionate staff at Osteoporosis and Rheumatology Center of Tampa Bay in Tampa, Florida is led by Jeffrey Miller, MD, a rheumatology and internal medicine specialist with years of experience in treating different types of pain. While you might think the pain youre feeling in your back means that you may have hurt your back, its possible that it could be your kidneys.
You May Like: Is Mio Bad For Your Kidneys
Treating Chronic Kidney Disease
There is no cure for chronic kidney disease, although treatment can slow or halt the progression of the disease and can prevent other serious conditions developing.
People with CKD are known to have an increased risk of a heart attack because of changes that occur to the circulation.
In a minority of people, CKD may cause kidney failure, also known as established renal failure or end-stage kidney disease. In this situation, the usual functions of the kidney stop working.
To survive, people with ERF may need to have artificial kidney treatment, called dialysis, or a kidney transplant.
Read more about living with chronic kidney disease
Reducing The Risk Of Developing Cardiovascular Diseases
People with chronic kidney disease have an increased risk of developing CVDs, such as heart disease, stroke, and peripheral arterial disease. People with CKD are actually twenty times more likely to die from cardiovascular-related problems than from kidney failure. This is why reducing any other cardiovascular risk factors is so important. See the separate leaflet called Cardiovascular Disease .
This typically includes:
Recommended Reading: Wine For Kidney Stones
Are There Stages Of Chronic Kidney Disease
Yes, there are five stages of kidney disease. The stages are based on how well your kidneys are able to do their job to filter out waste and extra fluid from your blood. The stages range from very mild to kidney failure . Healthcare providers determine the stage of your kidney function according to the glomerular filtration rate . Your GFR is a number based on the amount of creatinine, a waste product, found in your blood, along with other factors including your age, race and gender.
| Stages of Chronic Kidney Disease |
|---|
| Stage |
- Are African-American, Hispanic, Native American or Asian.
- Are over 60 years of age.
- Have a long history of taking painkillers, including over-the-counter products such as aspirin and ibuprofen.
Can Chronic Kidney Disease Be Prevented
Chronic kidney disease cannot be prevented in most situations. The patient may be able to protect their kidneys from damage, or slow the progression of the disease by controlling their underlying conditions such as diabetes mellitus and high blood pressure.
- Kidney disease is usually advanced by the time symptoms appear. If a patient is at high risk of developing chronic kidney disease, they should see their doctor as recommended for screening tests.
- If a patient has a chronic condition such as diabetes, high blood pressure, or high cholesterol, they should follow the treatment recommendations of their health care practitioner. The patient should see their health care practitioner regularly for monitoring. Aggressive treatment of these diseases is essential.
- The patient should avoid exposure to drugs especially NSAIDs , chemicals, and other toxic substances as much as possible.
Read Also: Can Kidney Infection Cause Diarrhea
Shortness Of Breath After Very Little Effort
Why this happens:
Being short of breath can be related to the kidneys in two ways. First, extra fluid in the body can build up in the lungs. And second, anemia can leave your body oxygen-starved and short of breath.
What patients said:
At the times when I get the shortness of breath, it’s alarming to me. It just fears me. I think maybe I might fall or something so I usually go sit down for awhile.
I couldn’t sleep at night. I couldn’t catch my breath, like I was drowning or something. And, the bloating, can’t breathe, can’t walk anywhere. It was bad.
What Is Kidney Failure
Kidney failure means that the kidneys have lost some of the capacity they have to filtrate the constituents in the plasma, the watery part of the blood. Conditions that can cause a decrease in this filtration capacity of the kidneys are:
- A fall in blood pressure
- A blockage of the blood that goes to the kidneys
- A blockage of the urine outflow
- Disease of the kidneys
- Kidney failure can be acute or chronic
Don’t Miss: Is Wine Bad For Kidney Stones
Swelling In Hands Or Feet
Why this happens:
Failing kidneys don’t remove extra fluid, which builds up in your body causing swelling in the legs, ankles, feet, and/or hands.
What patients said:
I remember a lot of swelling in my ankles. My ankles were so big I couldn’t get my shoes on.
Going to work one morning, my left ankle was swollen, real swollen, and I was very exhausted just walking to the bus stop. And I knew then that I had to see a doctor.
Kidney Disease: 11 Ways It Can Affect Your Skin
If you have kidney disease, you wont see early warning signs on your skin. However, as the disease progresses, you may develop one or more of the following:
Extremely dry skin. Skin can become so dry that it:
Itchy skin. Extremely itchy skin is a common symptom of advanced kidney disease. The itch can range from irritating to life-disrupting. Your skin may itch all the time.
Some people have itch on one area of their skin. The itch can also spread across most of your body.
Scratch marks and other signs of scratching. When you scratch often, it affects your skin. You can develop:
Color changes to your skin. When the kidneys stop working as they should, toxins build up in your body. This build-up can cause color changes to the skin. You may see any of the following:
Nail changes. Kidney disease can affect the appearance of your fingernails, toenails, or both. People who have advanced kidney disease can develop:
Read Also: Is Apple Cider Vinegar Good For Kidney Disease