The Need To Monitor Kidney Function With Certain Drugs
Experts have suggested that after the initial assessment of kidney function, physicians should consider regular monitoring after starting or increasing the dosage of drugs associated with nephrotoxicity, especially those used chronically in patients with multiple risk factors for impaired kidney function, Dr. Naughton noted. If there is any sign of kidney harm, the provider should review the medications you are taking in order to identify which one is causing the problem.
If multiple medications are present and the patient is clinically stable, physicians should start by discontinuing the drug most recently added to the patients medication regimen. Once that has been taken care of, further harm to the kidneys may be minimized by keeping blood pressure stable, staying hydrated, and temporarily avoiding the use of other medications that may cause nephrotoxicity.
These safety tips can ensure you get the care you need while keeping your kidneys safe. That way, they can tend to essential functions like keeping things flowing .Originally published May 11, 2017
What Are The Side Effects Of Diuretics And Can Diuretics Hurt My Kidneys
Dr. Hershberger answers the question: ‘Side Effects Of Diuretics?’
& #151 — Question: What are the side effects of diuretics, and can diuretics hurt my kidneys?
Answer: The side effects of diuretics are common. The most important by far is that they actually take too much fluid out of the body. As you know diuretics are designed to remove salt from the body, and with salt comes water. And sometimes too much of a diuretic effect can cause a patient to become too dry as we say — that can cause dizziness and light-headedness, and that can eventually, if it gets bad enough, cause some dysfunction of your kidneys.
Prescriptions Water Pills Can Be Helpful If Youre On Your Period
While itâs not recommended for healthy women to take any kind of water pills, there is one exception: to reduce period bloating. According to Anegawa, itâs fine for women to take prescription water pills to help de-puff unexplained leg swelling or bloating caused by PMS, says Anegawa.
Again, thatâs prescription-only, so donât head to your nearest drugstore for diuretics. Instead, bring up the issue to your ob-gyn, who may prescribe water pills to take before your period or whenever you tend to feel super-inflated. Since your physician will be keeping an eye on your dose, youâll reduce your risk of serious side effects and have someone to call if something feels off.
Donât Miss: Ginger Tea Dissolves Kidney Stones
Recommended Reading: Is It Ok To Drink Alcohol With Kidney Stones
Original Trial: Brief Description Of Protocol And Outcomes
The FACTT trial evaluated two fluid-management strategies in patients with ALI, randomizing 1000 ventilated patients in a two-by-two factorial design to either conservative or liberal fluid management and a pulmonary-artery or a central venous catheter for hemodynamic monitoring . The study protocols were approved by the institutional review board at each participating center, and the patients or their surrogates consented to study participation. The study design and results have been previously published .
Fluid management was directed for up to 7 days by a prespecified algorithm on the basis of on-study hemodynamic measurements. Intravascular pressure, measures of circulatory adequacy, and hourly urine-output measurements were used to determine administration of a fluid bolus or a diuretic, with lower intravascular pressures directing diuresis in the conservative arm compared with the liberal arm . The primary outcome of the original FACTT study was death by day 60. Secondary outcomes included renal failure within 7 and 28 days defined by the Brussels criteria, and dialysis requirement before day 60. There were no significant differences between fluid-management groups in mortality or the renal outcomes. Of note, patients in whom renal replacement therapy was planned or ongoing at screening were excluded. Enrollment into the trial occurred on average approximately 2 days after ICU admission.
Will Diuretics Cause Constipation
Yes, diuretics can cause constipation if you dont drink enough fluids.
A note from Cleveland Clinic
Diuretics can help you manage your high blood pressure and other conditions, but you need to take them the right way. Keep taking the same dose on schedule unless your provider tells you to change what youre doing. If the diuretic youre taking is giving you side effects, ask your provider if you can switch to a different diuretic.
Last reviewed by a Cleveland Clinic medical professional on 10/01/2021.
References
Recommended Reading: How To Test For Kidney Failure
Effect Of Neurohormonal Activation On Gfr
Reduced cardiac output causes neurohormonal activation. Sympathetic stimulation causes renal vasoconstriction and a fall in GFR. Increased activity of the RAAS causes glomerular arteriolar vasoconstriction that is more marked in the efferent than the afferent arteriole, helping to preserve GFR. Non-osmotic anti-diuretic hormone release contributes to hyponatraemia and also to increased urea reabsorption in the collecting duct: a disproportionate rise in blood urea is a marker of poor prognosis in patients with acute decompensated heart failure. Other neurohormones, particularly natriuretic peptides, counteract the effects of RAAS activation. GFR is also dependent on the vasodilator effects of prostaglandins. Non-steroidal anti-inflammatory drugs can therefore cause a marked fall in GFR.
Which Type Of Tea Causes Kidney Stones
Now, after knowing that green tea prevents the formation of kidney stones, you might be thinking that the effect is the same with other tea varieties as well. Arent you?
However, this is not true!
There are teas that cause kidney stones. Those who already suffer from kidney stones are not supposed to drink tea. This is because tea contains a high amount of oxalate that leads to the formation of kidney stones.
If you consume too much tea you can end up with kidney stones.
Now, as already discussed, green tea has a preventive effect with regard to kidney stones and this shows that not every tea causes them. It all depends on the oxalate level of tea.
When compared to green tea, black tea has a higher amount of oxalate present in it and therefore should be avoided.
P.S. It is still not very clear whether by bringing down your consumption of oxalate-rich foods you can prevent kidney stones or not. So, those with a history of kidney stones need to limit their consumption of food and drink that has more amount of oxalate.
You can always drink green tea as the amount of oxalate in it is quite less when compared to that of black tea.
Also Check: Is Ibuprofen Processed Through The Kidneys
Drug Dosing Adjustments In Patients With Chronic Kidney Disease
MYRNA Y. MUNAR, PHARMD, BCPS, and HARLEEN SINGH, PharmD, Oregon State University College of Pharmacy, Portland, Oregon
Am Fam Physician. 2007 May 15 75:1487-1496.
This article exemplifies the AAFP 2007 Annual Clinical Focus on management of chronic illness.
Chronic kidney disease affects renal drug elimination and other pharmacokinetic processes involved in drug disposition . Drug dosing errors are common in patients with renal impairment and can cause adverse effects and poor outcomes. Dosages of drugs cleared renally should be adjusted according to creatinine clearance or glomerular filtration rate and should be calculated using online or electronic calculators. Recommended methods for maintenance dosing adjustments are dose reductions, lengthening the dosing interval, or both. Physicians should be familiar with commonly used medications that require dosage adjustments. Resources are available to assist in dosing decisions for patients with chronic kidney disease.
The National Kidney Foundation Kidney Disease Outcomes Quality Initiative definition of chronic kidney disease is the presence of kidney damage or a reduction in the glomerular filtration rate for three months or longer. The K/DOQI chronic kidney disease staging system is based on GFR.1
SORT: KEY RECOMMENDATIONS FOR PRACTICE
SORT: KEY RECOMMENDATIONS FOR PRACTICE
National Kidney Foundation K/DOQI Staging System for Chronic Kidney Disease
|
Publisher: American College of Physicians |
How Can Diuretics For Hypertension Affect Your Kidney Function
When it comes to the treatment of hypertension, one of the first types of drugs that a family practitioner or cardiologist will prescribe is going to be a diuretic. You may have heard of diuretics, which are more commonly described as water pills”, before. When the kidneys are working properly, these medications can work wonders by influencing how elements like sodium, potassium and chlorine are absorbed within the kidney apparatus. As these elements are secreted into the kidney tract, water is likely to follow. As a result, a person taking diuretics will essentially be removing excessive water from their body.
Also Check: Does Potassium Citrate Dissolve Kidney Stones
When Will I Take It
Itâs usual to take furosemide once a day in the morning.
Sometimes you take it twice a day once in the morning and again at lunchtime. Occasionally, you take it every other day.
You donât need to take furosemide at the same time every day. You can occasionally take it at a different time if itâs more convenient for you, for example if you need to go out for a few hours in the morning and you wonât be near a toilet.
But do not take furosemide too late in the day or at night, otherwise you may have to wake up to go to the toilet. Your doctor or pharmacist will tell you the best times for you to take your medicine.
Talk With Your Doctor
Prescription diuretics can be helpful in treating serious conditions, such as heart failure, to less-pressing conditions, such as mild high blood pressure.
If your doctor prescribes a diuretic, feel free to ask them any questions you may have. Consider discussing these questions:
- How will I know my diuretic is working the way its supposed to work?
- Am I taking any medications that might interact with a diuretic?
- Should I follow a low-salt diet while taking a diuretic?
- Should I have my blood pressure and kidney function tested while taking this drug?
- Should I take a potassium supplement or avoid foods that contain potassium?
Read Also: Does Kidney Disease Cause Rashes
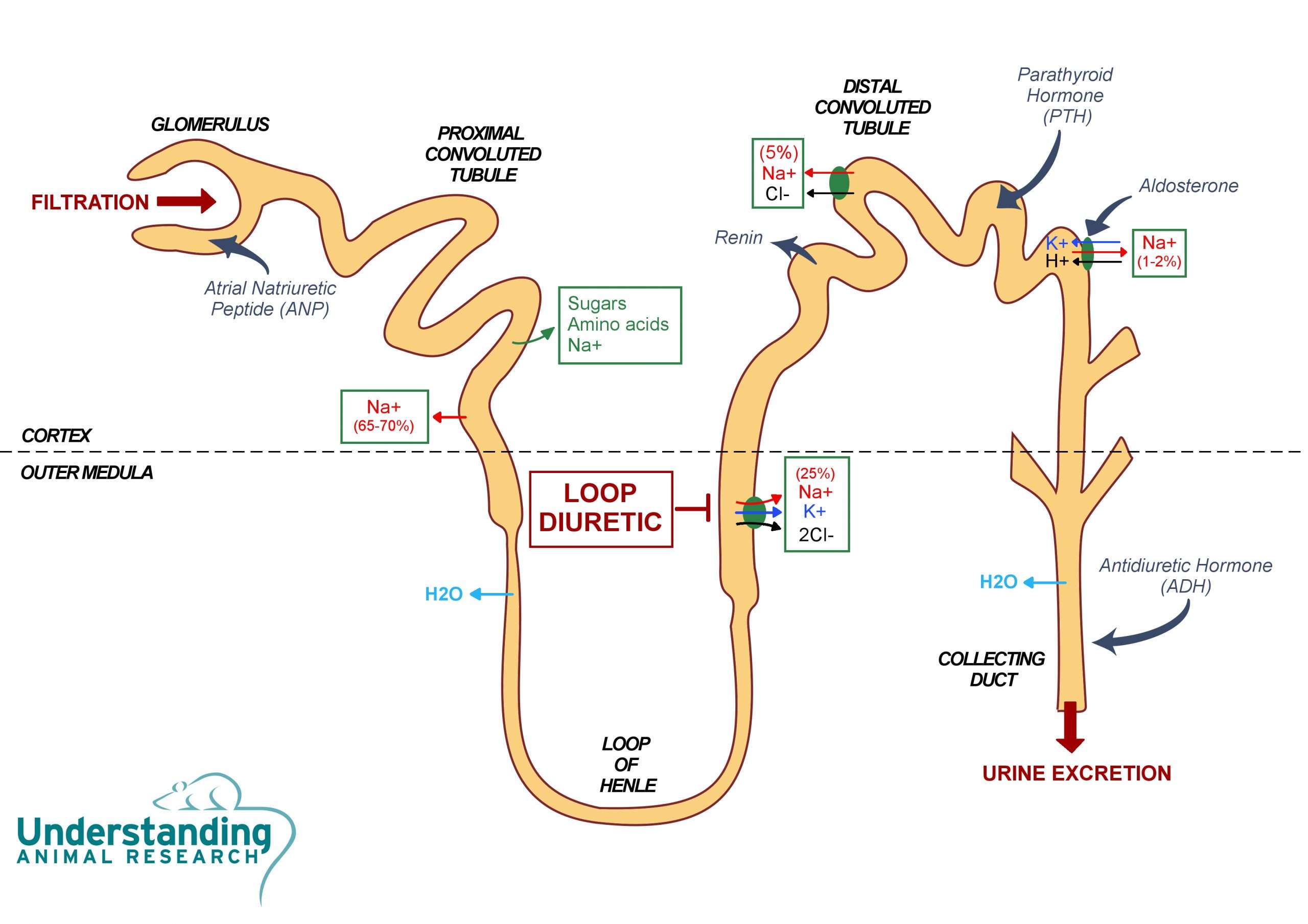
What Are Diuretics And How Do They Work
The amount of fluid retained by the body is controlled primarily by the kidneys. This occurs due to the kidneyâs ability to control the retention and elimination of sodium and chloride because the amounts of sodium, chloride, and water in the body are carefully balanced. Thus, if sodium and chloride are eliminated from the body, water also is eliminated. Conversely, if sodium and chloride are retained by the body, so is water.
The elimination of sodium, chloride, and water from the body is somewhat complex. In the kidneys, sodium, chloride, and other small molecules are filtered out of the blood and into the tubules of the kidney where urine is formed. Most of the sodium, chloride, and water are reabsorbed into the blood before the filtered fluid leaves the kidney in the form of urine. To make matters even more complex, there are different mechanisms that are active in different parts of the tubules that affect the reabsorption of sodium and chloride.
Diuretics are a class of drugs that increase the flow of urine . Diuretics work by removing sodium and chloride from the body in the urine, and the sodium and chloride, in turn, draw excess water from the body.
- The amount of sodium and chloride in the body, as previously discussed, has a marked effect on the amount of water retained by the body hence most diuretics have their effects by reducing total-body sodium chloride content.
You May Like: Kidney Pain High Blood Pressure
Are Your Medications Causing Kidney Disease
Duncan Capicchiano
No matter what kind of medication you take, whether over-the-counter or prescription, it is destined to take a trip through your kidneys. Because the kidneys provide the final pathway for excreting drugs and their metabolites, they are unfortunately subjected to high concentrations of potentially toxic substances.
Medications that can damage the kidneys are known as nephrotoxic medications. Some of these medications mildly worsen kidney function, others can cause acute kidney injury or lasting kidney damage.
Drugs cause nephrotoxicity in different ways but their main effects can be grouped into four categories:
The risk for kidney damage depends on your individual health and other medications you are taking. People with existing kidney conditions or damage are at much greater risk of harm by nephrotoxic medications.
Don’t Miss: What Type Of Doctor Do You See For Kidney Stones
Avoiding The Triple Whammy
The term triple whammy refers to the use of an ACE inhibitor or angiotensin-II receptor blocker , with a diuretic and a NSAID.
ACE inhibitors or ARBs and diuretics are commonly prescribed together however taking these medications together can increase the risk of AKI. Prescribing a NSAID alongside these medications considerably increases the risk of AKI.
Effects Of Renal Artery Stenosis And Intrarenal Vascular Disease
Angiotensin II causes a preferential increase in efferent arteriolar tone, helping to maintain GFR when afferent arteriolar pressure is low, as in renal artery stenosis and severe generalised intrarenal arteriosclerosis. In these settings, inhibition of angiotensin II production by ACEI or ARB can lead to acute renal failure, which is not always reversible.
Also Check: Can Taking Creatine Cause Kidney Problems
What Drugs Interact With Lasix And Thiazide Diuretics
Lasix
- Administration of Lasix with aminoglycoside antibiotics or ethacrynic acid may cause hearing damage.
- Lasix competes with aspirin for elimination in the urine by the kidneys. Concomitant use of furosemide and aspirin may, therefore, lead to high blood levels of aspirin and aspirin toxicity.
- Lasix also may reduce excretion of lithium by the kidneys, causing increased blood levels of lithium and possible side effects from lithium.
- Sucralfate reduces the action of Lasix by binding Lasix in the intestine and preventing its absorption into the body. Ingestion of Lasix and sucralfate should be separated by two hours.
- When combined with other antihypertensive drugs, there is an increased risk of low blood pressure or reduced kidney function.
- Nonsteroidal anti-inflammatory drugs â for example., ibuprofen, indomethacinâ may interfere with the blood pressure-reducing effect of Lasix.
Thiazide diuretics
You May Like: Osteocleanse
Congestion In Heart Failure
It has been difficult to demonstrate a uniform benefit with respect to any individual therapeutic intervention in patients with AHF . This is probably due to a wide range of pathophysiologies that result in a common phenotypic appearance of pulmonary congestion and peripheral edema . Although pulmonary and systemic congestion may be the most overt findings, these may be the tip of the iceberg reflecting significant congestion of multiple organs, including the kidneys. Many cardiac and extracardiac factors can lead to congestion: left ventricular adverse remodeling, hypertrophy, and stiffness coronary artery disease and microvascular ischemia decreased systemic vascular compliance reduced venous capacitance and excessive preload superimposed right ventricular dysfunction and pulmonary hypertension. Neurohormonal determinants include renin-angiotensin activation, nervous sympathetic overdrive, increased arginine-vasopressin activity, endothelin secretion, and increased immune cell signaling. Clinically, the patient with AHF can be categorized into a two-by-two table according to good or poor systemic perfusion and to the presence or absence of congestion . Those with both poor perfusion and congestion have the worst overall risk for short- and long-term mortality as well as worsened renal function after the initiation of intravenous loop diuretics.
Fig. 1
You May Like: How Do You Diagnose A Kidney Infection
Electrolyte Imbalance And Other Side Effects
The 2020 JAMA study isnt the first study to find side effects with chlorthalidone, according to Columbia University. Previous studies found that the drug was associated with more electrolyte imbalances than hydrochlorothiazide.
Electrolyte balance refers to the balance between sodium, calcium, potassium, chloride, phosphate and magnesium in the body. Too little or too much water in the body can cause these levels to become imbalanced and lead to several side effects.
According to the Thalitone drug label, all patients taking chlorthalidone should be observed for clinical signs of electrolyte imbalance, including:
- Drowsiness
- Gastrointestinal disturbances, such as nausea and vomiting
- Lethargy
Characteristics Of Participants Experiencing Aki
Of the 1000 FACTT participants, 306 developed stage 1 or worse AKI within 2 study days of enrollment. Slightly more participants were in the fluid-conservative arm than the fluid-liberal arm . Most developed stage 1 AKI. Baseline and on-study characteristics of included participants, stratified by fluid-management strategy, are shown in . The groups were similar with the exception of baseline albumin levels, fluid balance in the 24 hours prerandomization, and proportion with aspiration as an etiology of ALI. There was no significant difference in mortality rate or time to death between the two groups.
Characteristics of FACTT participants with AKI, comparing those randomized to the liberal-fluid strategy with those randomized to the restrictive strategy
Read Also: Can Sweet Tea Cause Kidney Stones
While Youre Taking Diuretics
Let your doctor know what medications , supplements, and herbal remedies you use. Also, tell them about other medical problems you have.
They may want to regularly check your blood pressure as well as test your blood and pee for levels of specific minerals and to see how well your kidneys are working. Theyâll probably tell you to follow a low-sodium diet and limit how much salt you eat.
Because some diuretics also pull potassium out of your body, you might need to eat more foods like bananas, sweet potatoes, spinach, and lentils, or take a potassium supplement. On the other hand, if youâre taking a âpotassium-sparingâ diuretic, such as amiloride , spironolactone , or triamterene , they may want you to avoid potassium-rich foods, salt substitutes, low-sodium milk, and other sources of potassium.
If you only need one dose a day, you might want to take your diuretic in the morning so you can sleep through the night instead of getting up to go to the bathroom.
Avoid alcohol and medicines to help you sleep. They may make side effects worse.
You May Like: Kidney Sickness Symptoms