Pathophysiology Of Fluid Retention In Cirrhosis
In cirrhosis, disturbances in fluid balance precede ascites formation by several weeks. In this phase, intravascular volume expansion results from renal sodium retention.140 Renal tubular sodium retention also precedes changes in renal blood flow, GFR, filtration fraction, and intrarenal vascular resistance associated with cirrhosis.127 A 36% plasma volume expansion occurred in cirrhotic dogs during this active salt-retaining, preascitic phase, with two thirds of the newly acquired volume distributed to the vasodilated splanchnic circulation.126 Ascites formation is hastened by sodium ingestion or intravenous administration of sodium-containing fluids. Surgical creation of portosystemic shunting in dogs with hepatic cirrhosis abolished portal hypertension and the early tendency for renal sodium retention and ascites. In such studies, 20- to 30-lb cirrhotic dogs with shunts were able to maintain normal sodium balance with intakes as high as 85 mEq/day. Cirrhotic dogs without shunts accumulated sodium at this level of intake.225
Peripheral arterial and splanchnic vasodilatation initiates water and sodium conservation in cirrhosis.90 Peripheral arterial vasodilatation reenforces the signal initiating renal sodium retention . The physiologic responses observed after acute portal vein constriction are similar to those associated with the hyperdynamic circulatory syndrome of cirrhosis.21
Ang Iimediated Changes In Peritubular Capillary Dynamics Promote Increased Tubular Reabsorption
Ang IImediated constriction of efferent arterioles stabilizes GFR, but also reduces renal blood flow and peritubular capillary hydrostatic pressure, and increases peritubular colloid osmotic pressure as a result of increased filtration fraction.18 These changes, in turn, reduce the hydrostatic pressure of renal interstitial fluid and raise interstitial fluid colloid osmotic pressure, thereby increasing the driving force for fluid reabsorption across tubular epithelial cells and reducing back-leak of sodium from the intercellular spaces into the tubules.
The effects of Ang II on renal hemodynamics and interstitial fluid dynamics may also alter reabsorption in more distal parts of the tubule. For example, reductions in renal medullary blood flow due to efferent arteriolar constriction or to direct effects of Ang II on the vasa recta may enhance reabsorption in the loop of Henle and collecting ducts.18,34 Thus, there are several pathways by which subtle changes in renal hemodynamics, without major changes in GFR, may mediate the effects of Ang II to enhance renal sodium reabsorption.
M. Gupta, in, 2010
Blood Filtration And Nutrient And Water Reabsorption
Kidneys filter blood in a three-step process. First, the nephrons filter blood that runs through the capillary network in the glomerulus. Almost all solutes, except for proteins, are filtered out into the glomerulus by a process called glomerular filtration. Second, the renal tubules collect the filtrate. Most of the solutes are reabsorbed in the PCT by a process called tubular reabsorption. In the loop of Henle, the filtrate continues to exchange solutes and water with the renal medulla and the peritubular capillary network.
Nephron structure
Finally, some substances, such as electrolytes and drugs, are removed from blood through the peritubular capillary network into the distal convoluted tubule or collecting duct. Urine is a collection of substances that have not been reabsorbed during glomerular filtration or tubular reabsorbtion.
Also Check: Is Cranberry Juice Good For Your Liver And Kidneys
How Do My Kidneys Work
Each of your kidneys is made up of about a million filtering units called nephrons. Each nephron includes a filter, called the glomerulus, and a tubule. The nephrons work through a two-step process: the glomerulus filters your blood, and the tubule returns needed substances to your blood and removes wastes.
Reabsorption Moves Nutrients And Water Back Into The Bloodstream
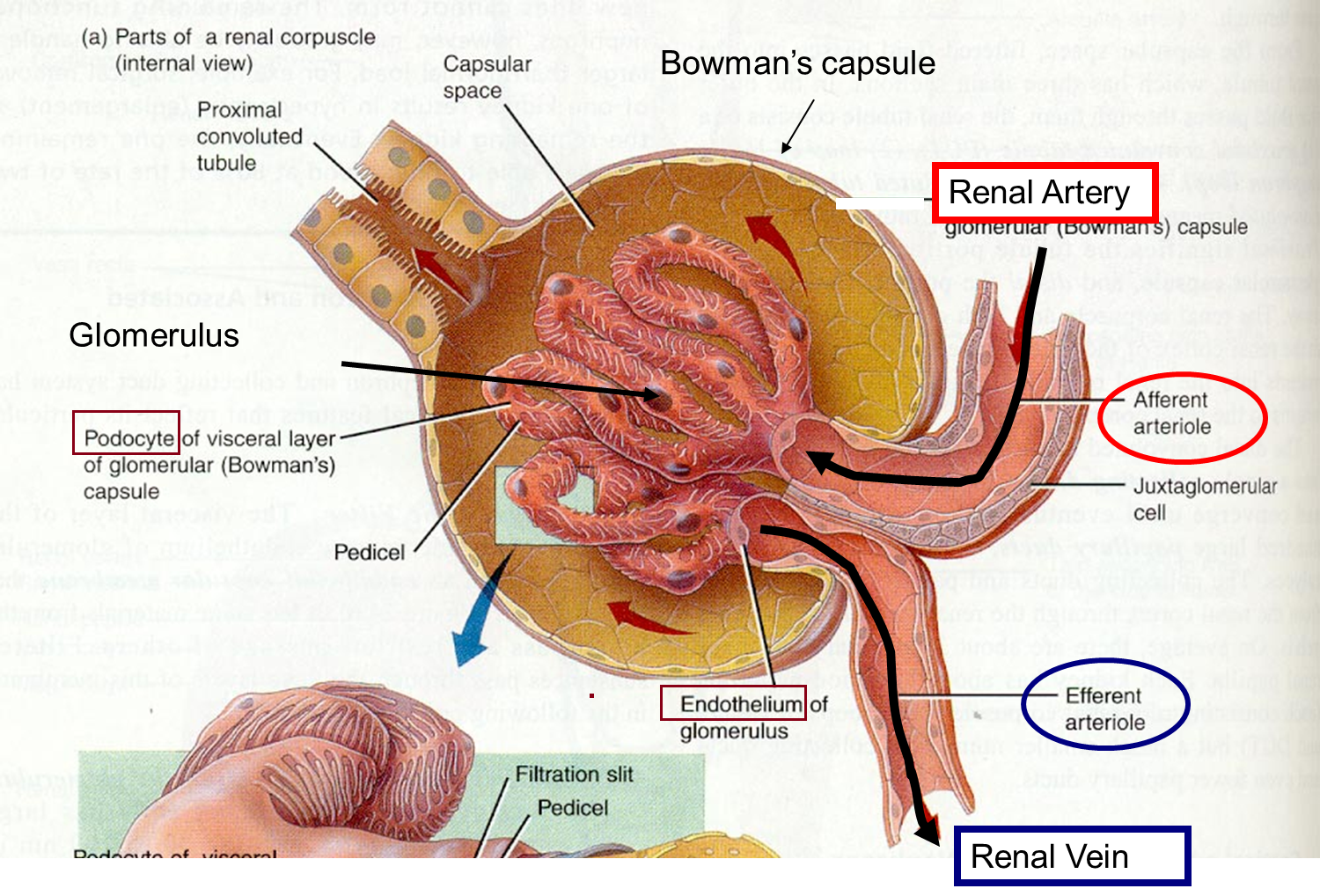
The glomerulus filters water and small solutes out of the bloodstream. The resulting filtrate contains waste, but also other substances the body needs: essential ions, glucose, amino acids, and smaller proteins. When the filtrate exits the glomerulus, it flows into a duct in the nephron called the renal tubule. As it moves, the needed substances and some water are reabsorbed through the tube wall into adjacent capillaries. This reabsorption of vital nutrients from the filtrate is the second step in urine creation.
Read Also: Does Pellegrino Cause Kidney Stones
Water And Electrolyte Balance
People consume water regularly in order to maintain life. More water is produced by the processing of food. If the amount of water added to the body is not matched by an equal amount going out, water accumulates rapidly and the person becomes ill and may even die. Excess water dilutes the body’s electrolytes, whereas water restriction concentrates them. The body’s electrolytes must be maintained at very precise concentrations. The kidneys regulate and help maintain the proper balance of water and electrolytes.
Blood enters a glomerulus at high pressure. Much of the fluid part of blood is filtered through small pores in the glomerulus, leaving behind blood cells and most large molecules, such as proteins. The clear, filtered fluid enters Bowman space and passes into the tubule leading from Bowman capsule. In healthy adults, about 47 gallons of fluid is filtered into the kidney tubules each day. Nearly all this fluid is reabsorbed by the kidney. Only about 1.5 to 2% of the fluid is excreted as urine. For this reabsorption to occur, different parts of the nephron actively secrete and reabsorb different electrolytes, which pull the water along, and other parts of the nephron vary their permeability to water, allowing more or less water to return to the circulation. The details of these processes are a bit complicated.
Function Of A Nephron
The simplified diagram of a nephron in Figure 16.4.6 shows an overview of how the nephron functions. Blood enters the nephron through an arteriole called the afferent arteriole. Next, some of the blood passes through the capillaries of the glomerulus. Any blood that doesnt pass through the glomerulus as well as blood after it passes through the glomerular capillaries continues on through an arteriole called the efferent arteriole. The efferent arteriole follows the renal tubule of the nephron, where it continues playing a role in nephron functioning.
Also Check: Is Pomegranate Juice Good For Kidneys
Regulation Of Blood Pressure
Another function of the kidneys is to help regulate the body’s blood pressure by excreting excess sodium. If too little sodium is excreted, blood pressure is likely to increase. The kidneys also help regulate blood pressure by producing an enzyme called renin. When blood pressure falls below normal levels, the kidneys secrete renin into the bloodstream, thereby activating the renin-angiotensin-aldosterone system Regulating Blood Pressure: The Renin-Angiotensin-Aldosterone System High blood pressure is persistently high pressure in the arteries. Often no cause for high blood pressure can be identified, but sometimes it occurs as a result of an underlying… read more , which in turn raises blood pressure. The kidneys also produce urotensin, which causes blood vessels to constrict and helps raise blood pressure. A person with kidney failure is less able to regulate blood pressure and tends to have high blood pressure.
The Tubule Returns Needed Substances To Your Blood And Removes Wastes
A blood vessel runs alongside the tubule. As the filtered fluid moves along the tubule, the blood vessel reabsorbs almost all of the water, along with minerals and nutrients your body needs. The tubule helps remove excess acid from the blood. The remaining fluid and wastes in the tubule become urine.
Recommended Reading: Can Pepsi Cause Kidney Stones
What Are The Kidneys And Urinary Tract
The urinary tract is one of the systems that our bodies use to get rid of waste products. The kidneys are the part of the urinary tract that makes urine . Urine has salts, toxins, and water that need to be filtered out of the blood. After the kidneys make urine, it leaves the body using the rest of the urinary tract as a pathway.
Effects Of Other Cardiovascular Drugs On Renal Function
Angiotensin II is one of the factors responsible for efferent arteriolar vasoconstriction and increased filtration fraction in CHF. The ACE inhibitors, such as enalapril, may antagonize efferent arteriolar constriction sufficiently in some patients to cause an abrupt decrease in glomerular perfusion pressure. This effect is especially likely in volume-depleted patients. The result is acute renal failure, with serum creatinine concentration often exceeding 5 mg/dL. Renal failure in this setting generally can be reversed by reducing diuretic dosage, decreasing the dosage of the ACE inhibitor, and providing judicious fluid therapy . After volume repletion, the dosage of the ACE inhibitor is increased over 2 to 4 weeks, and the drug combination is adjusted while monitoring body weight, clinical signs of CHF, ABP, and serum creatinine concentration.
Stephen P. DiBartola, in, 2012
Recommended Reading: Does Red Wine Cause Kidney Stones
With Chronic Kidney Disease
With kidney disease, risk of nutrient, toxin, and waste build up is higher. More specifically, damage to kidneys can lead to damage of the filtering process. Consequently, larger items like protein leak into the urine.
This is where specific diets are important. More specifically, the different stages can result in different diet, medication, and lifestyle needs for each person.
Taking kidney cleansing vitamins are not helpful. When the kidneys arent working, they wont get rid of the excess.
What Are The Two Components Of The Nephron
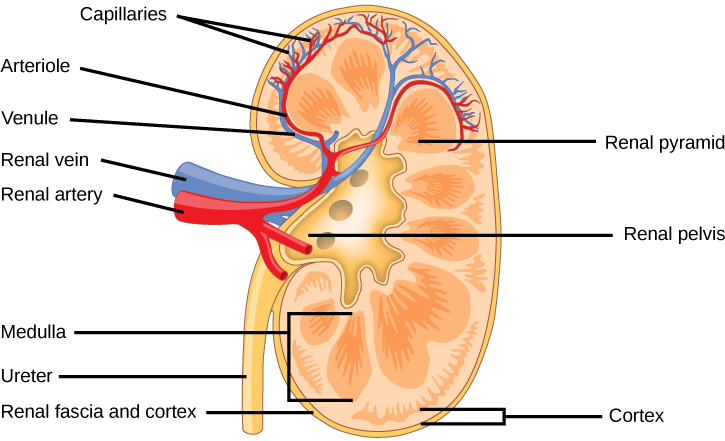
The nephron consists of the renal corpuscle and the renal tubule. The nephron is responsible for filtration, excretion and resorption. It filters out small molecules from plasma, selectively re-absorbs most of the water, and some of the molecules, and also secretes some secretory products into the filtrate.
Don’t Miss: Kidney Transplant Tattoos
Processes Of The Kidneys
Filtration
Filtration is the mass movement of water and solutes from plasma to the renal tubule that occurs in the renal corpuscle. About 20% of the plasma volume passing through the glomerulus at any given time is filtered. This means that about180 liters of fluid are filtered by the kidneys every day. Thus, the entire plasma volume is filtered 60 times a day! Filtration is primarily driven by hydraulic pressure in the capillaries of the glomerulus.
Note that the kidneys filter much more fluid than the amount of urine that is actually excreted . This is essential for the kidneys to rapidly remove waste and toxins from the plasma efficiently.
Reabsorption
Reabsorption is the movement of water and solutes from the tubule back into the plasma. Reabsorption of water and specific solutes occurs to varying degrees over the entire length of the renal tubule. Bulk reabsorption, which is not under hormonal control, occurs largely in the proximal tubule. Over 70% the filtrate is reabsorbed here. In addition, many important solutes are actively transported out of the proximal tubule such that their concentrations are normally extremely low in the remaining fluid. Further bulk reabsorption of sodium occurs in the loop of Henle.
Regulated reabsorption, in which hormones control the rate of transport of sodium and water depending on systemic conditions, takes place in the distal tubule and collecting duct.
Secretion
Excretion
Waste Ions And Hydrogen Ions Secreted From The Blood Complete The Formation Of Urine
The filtrate absorbed in the glomerulus flows through the renal tubule, where nutrients and water are reabsorbed into capillaries. At the same time, waste ions and hydrogen ions pass from the capillaries into the renal tubule. This process is called secretion. The secreted ions combine with the remaining filtrate and become urine. The urine flows out of the nephron tubule into a collecting duct. It passes out of the kidney through the renal pelvis, into the ureter, and down to the bladder.
Don’t Miss: Is Grape Juice Good For Kidney Stones
So Why Are Kidneys Important
As weve seen, the kidney clearly has very important jobs in the body. Some of these functions can decline with or without symptoms in kidney disease.
If you have kidney disease, you may need help with changes in medical care, medications, diet, and lifestyle. Talk with your healthcare team about what you can do as a team to keep your kidneys working.
Struggling with kidney disease? Want to learn more about the kidney diet and kidney-friendly nutrition? Check out our Plant-Powered Kidneys online course!
Overview Of Kidney Filtering Disorders
, MD, Washington University in St. Louis
Each kidney contains about 1 million filtering units . The glomeruli are made up of many microscopic clusters of tiny blood vessels with small pores. These blood vessels are designed to leak fluid from the bloodstream into a system of miniature tubules. The tubules secrete and reabsorb chemicals and substances from the fluid to cause it to become urine. The urine then drains from the tubules into larger and larger tubes until it leaves the kidney. Normally this filtering system permits fluid and small molecules … read more ) to leak into the tubules. Diseases that affect the kidneys can be divided into three categories based on the way they affect different parts of the kidneys:
-
Glomerulonephritis is inflammation of the glomeruli, which causes blood cells and protein to escape from the glomerular capillaries into the urine and is sometimes hereditary disorder that results in glomerulonephritis in which kidney function is poor, blood is present in the urine, and deafness and eye abnormalities sometimes… read more ).
-
Nephrotic syndrome occurs when damage to the capillaries of the glomeruli causes proteins to leak into the urine.
-
Tubulointerstitial nephritis is inflammation of the tubules and/or the tissues surrounding the tubules .
Some disorders have features of both glomerulonephritis and nephrotic syndrome.
Read Also: Does Pop Cause Kidney Stones
The Glomerulus Filters Water And Other Substances From The Bloodstream
Each kidney contains over 1 million tiny structures called nephrons. Each nephron has a glomerulus, the site of blood filtration. The glomerulus is a network of capillaries surrounded by a cuplike structure, the glomerular capsule . As blood flows through the glomerulus, blood pressure pushes water and solutes from the capillaries into the capsule through a filtration membrane. This glomerular filtration begins the urine formation process.
What Clinical Trials Are Open
Clinical trials that are currently open and are recruiting can be viewed at www.ClinicalTrials.gov.
This content is provided as a service of the National Institute of Diabetes and Digestive and Kidney Diseases, part of the National Institutes of Health. The NIDDK translates and disseminates research findings to increase knowledge and understanding about health and disease among patients, health professionals, and the public. Content produced by the NIDDK is carefully reviewed by NIDDK scientists and other experts.
Recommended Reading: Can Seltzer Water Cause Kidney Stones
Feature: Human Biology In The News
Kidney failure is a complication of common disorders including diabetes mellitus and hypertension. It is estimated that approximately 12.5% of Canadians have some form of kidney disease. If the disease is serious, the patient must either receive a donated kidney or have frequent hemodialysis, a medical procedure in which the blood is artificially filtered through a machine. Transplant generally results in better outcomes than hemodialysis, but demand for organs far outstrips the supply. The average time on the organ donation waitlist for a kidney is four years. There are over 3,000 Canadians on the wait list for a kidney transplant and some will die waiting for a kidney to become available.
For the past decade, Dr. William Fissell, a kidney specialist at Vanderbilt University, has been working to create an implantable part-biological and part-artificial kidney. Using microchips like those used in computers, he has produced an artificial kidney small enough to implant in the patients body in place of the failed kidney. According to Dr. Fissell, the artificial kidney is a bio-hybrid device that can mimic a kidney to remove enough waste products, salt, and water to keep a patient off dialysis.
Kidneys Are A Filter System
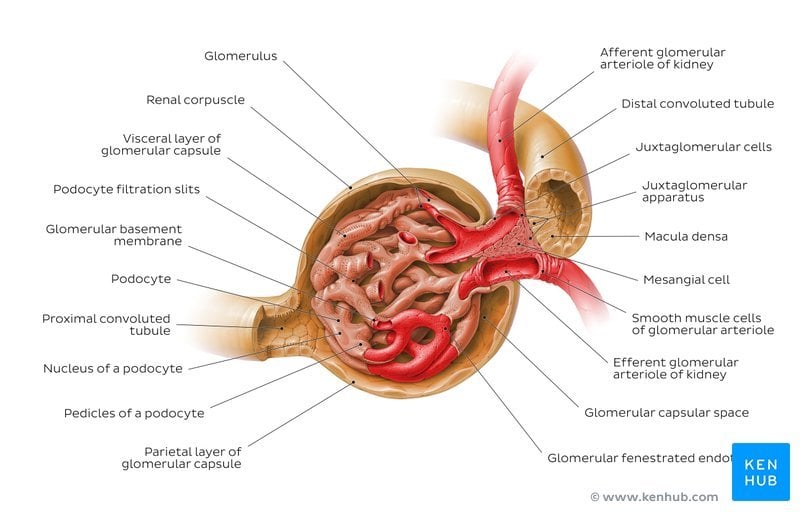
The main job of the kidneys is to remove waste from the blood and return the cleaned blood back to the body. Each minute about one litre of blood one-fifth of all the blood pumped by the heart enters the kidneys through the renal arteries. After the blood is cleaned, it flows back into the body through the renal veins.
Each kidney contains about one million tiny units called nephrons. Each nephron is made up of a very small filter, called a glomerulus, which is attached to a tubule. As blood passes through the nephron, fluid and waste products are filtered out. Much of the fluid is then returned to the blood, while the waste products are concentrated in any extra fluid as urine .
The urine flows through a tube called the ureter into the bladder. Urine passes from the bladder out of the body through a tube called the urethra. The kidney usually makes one to two litres of urine every day depending on your build, how much you drink, the temperature and the amount of exercise you do.
A healthy kidney can greatly increase its work capacity. With two healthy kidneys, each kidney performs 50 per cent of the normal kidney function. If one kidney is lost, the other kidney can enlarge and provide up to 75 per cent of the normal kidney function .
Also Check: Is Red Wine Bad For Kidney Stones
What Is The Function Of Nephrons Answers
Its function is to produce urine and remove waste and excess substances from the blood. Complete Answer: Nephron is the structural and functional unit of Kidney. Its main function is to convert blood into urine by filtration, reabsorption, secretion and excretion of useful and harmful substances present in the blood.
Renal Pelvis And Ureter
Numerous collecting ducts merge into the renal pelvis, which then becomes the ureter. The ureter is a muscular tube, composed of an inner longitudinal layer and an outer circular layer. The lumen of the ureter is covered by transitional epithelium . Recall from the Laboratory on Epithelia that the transitional epithelium is unique to the conducting passages of the urinary system. Its ability to stretch allows the dilation of the conducting passages when necessary. The ureter connects the kidney and the urinary bladder.
Recommended Reading: Is Seltzer Water Bad For Your Kidneys