Autosomal Recessive Polycystic Kidney Disease
NORD gratefully acknowledges Peter C. Harris, PhD, Professor Biochemistry/Molecular Biology and Medicine, Division of Nephrology and Hypertension, Mayo Clinic, for assistance in the preparation of this report.
Synonyms of Autosomal Recessive Polycystic Kidney Disease
- ARPKD
- polycystic kidney disease, infantile
General Discussion
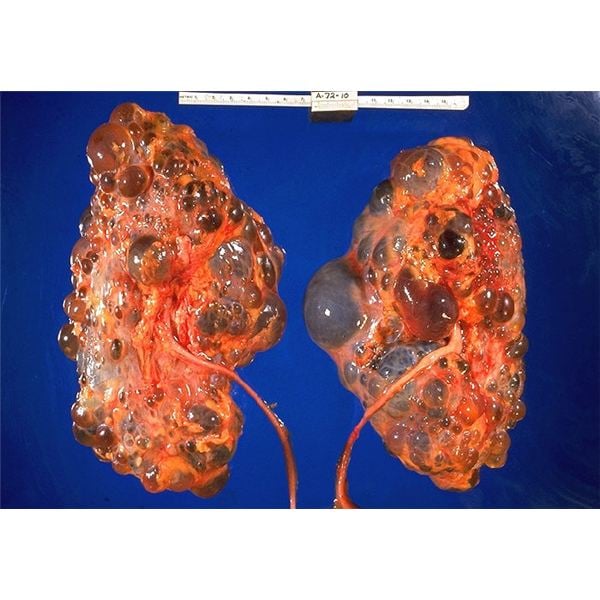
Autosomal recessive polycystic kidney disease is a rare genetic disorder characterized by the formation of fluid-filled sacs in the kidneys. Most affected infants have enlarged kidneys during the newborn period and some cases may be fatal at this time. ARPKD is not simply a kidney disease and additional organ systems of the body may also be affected, especially the liver. High blood pressure , excessive thirst, frequent urination and feeding difficulties may also occur. Some affected children may also have distinctive facial features and incomplete development of the lungs causing breathing difficulties. The severity of the disorder and the specific symptoms that occur can vary greatly from one person to another. Some affected children eventually develop end-stage renal disease sometime during the first decade of life. In some patients, symptoms do not develop until adolescence or even adulthood. ARPKD is caused by changes in the PKHD1 gene.
Signs & Symptoms
Causes
ARPKD is caused by mutations of the PKHD1 gene and is inherited in an autosomal recessive pattern.
Affected Populations
Related Disorders
Diagnosis
Standard Therapies
Treatment
References
What Is The Treatment For Polycystic Kidney Disease
The most common treatments for PKD include:
- Blood pressure management: Your provider helps you control your blood pressure with medicine, diet and exercise. Keeping your blood pressure within a safe range reduces your risk of heart disease and stroke.
- Breathing support: Infants with underdeveloped lungs and breathing problems may need mechanical ventilation.
- Dialysis: If you have kidney failure, you may need dialysis . Hemodialysis uses a machine to filter blood outside the body. Peritoneal dialysis uses the lining of your belly and a special fluid to filter blood.
- Growth therapy: Underweight or underdeveloped infants may need help growing. A healthcare provider may recommend nutritional therapy or human growth hormone.
- Kidney transplant: You may need a kidney transplant if ADPKD progresses to end-stage renal failure. A transplant is surgery to replace a failing kidney with a donor kidney.
- Pain management: Medicine can control pain caused by infections, kidney stones or burst cysts. Your healthcare provider should approve any pain medicines you take. Some medicines can make kidney damage worse.
How Is Pkd Diagnosed
Because ADPKD and ARPKD are inherited, your doctor will review your family history. They may initially order a complete blood count to look for anemia or signs of infection and a urinalysis to look for blood, bacteria, or protein in your urine.
To diagnose all three types of PKD, your doctor may use imaging tests to look for cysts of the kidney, liver, and other organs. Imaging tests used to diagnose PKD include:
- Abdominal ultrasound. This noninvasive test uses sound waves to look at your kidneys for cysts.
- Abdominal CT scan. This test can detect smaller cysts in the kidneys.
- Abdominal MRI scan. This MRI uses strong magnets to image your body to visualize kidney structure and look for cysts.
- Intravenous pyelogram. This test uses a dye to make your blood vessels show up more clearly on an X-ray.
In addition to the symptoms generally experienced with PKD, there may be complications as cysts on the kidneys grow larger.
These complications may include:
- diuretics to help remove excess fluid from the body
- surgery to drain cysts and help relieve discomfort
In 2018, the Food and Drug Administration approved a drug called tolvaptan as a treatment for ADPKD. Its used to slow the progression of kidney decline.
One of the serious potential side effects of tolvaptan is severe liver damage, so your doctor will regularly monitor the health of your liver and kidneys while on this medication.
Reaching out to a support network of family and friends can be helpful.
Don’t Miss: Can Pepsi Cause Kidney Stones
Risk Factors For Cardiovascular Disease
High blood pressure is the second leading cause of Chronic Kidney Disease because it can damage blood vessel walls over time. This can decrease the amount of oxygen that can get to organs like the kidneys and heart. The high pressure can also damage the tiny filters inside the kidneys which clean our blood. If a person with CKD develops high blood pressure it is more likely that their kidney disease will get worse and they will have heart problems Cardiovascular Disease .
Anemia occurs when there are not enough red blood cells to carry oxygen to organs and cells. Healthy kidneys produce a hormone called erythropoietin which helps to produce red blood cells. Damaged kidneys make less EPO so people with CKD produce fewer red blood cells and less oxygen is carried. This causes the heart to work harder to circulate the oxygen needed by the other organs and cells which can cause CVD.
Abnormal calcium and phosphorus levels can lead to CKD-MBD . Early in CKD there can be changes in how the body balances calcium and phosphorus. Extra phosphorus and calcium may be removed from the bones and be deposited in blood vessels and organs. These bone-like deposits damage blood vessels and organs like the heart, leading to CVD.
Tips On How To Suspect An Ikd
Although, as previously pointed out, a significant percentage of patients with kidney disease of unknown aetiology may have an IKD and genetic testing allows a diagnosis to be made, one must not make the mistake of requesting unsubstantiated genetic studies. While the cost of NGS has decreased, it is still sufficiently high that it must not be used in a non-cost-effective way.
The following circumstances may arouse suspicion of an IKD, in descending order of importance :
Situations warranting suspicion of an IKD.
-
a family history of kidney disease or a patient from an area with a high level of inbreeding, which may make one think of an autosomal recessive disease
-
patients with cystic kidney diseases, tubulopathies or suspected monogenic glomerulopathies have a likely monogenic cause of the disease
-
a syndromic disease in which organs besides the kidney are affected
-
congenital kidney anomalies
-
kidney disease of unknown aetiology in patients < 2530years of age at least 20% of CKD patients under the age of 25 years have an IKD
-
haematuric kidney disease without a definitive diagnosis by kidney biopsy or with a diagnosis of FSGS such disease may be due to mutations in the COL4A3 or COL4A4 genes, giving rise to the so-called autosomal dominant Alport syndrome with highly variable clinical expression
-
interstitial nephropathy without an apparent cause, even in the absence of a family history, as it may show incomplete penetrance or be a sporadic case.
Also Check: Is Wine Bad For Kidney Stones
Gene Identification Informs Diagnostics Therapy And Pathogenesis
A very important feature of monogenic diseases is the fact that the mutation in itself represents the primary cause of the disease. This provides the following opportunities for diagnostics, therapy, and insights into pathogenesis: i) Unequivocal molecular genetic diagnostics can be performed to avoid invasive procedures, e.g. the diagnosis of nephronophthisis can be made without the necessity for renal biopsy. ii) Prenatal diagnosis is possible, e.g. for diagnostics of the perinatal lethal Meckel-Gruber syndrome. iii) Specific prognostic outcomes can be delineated for specific mutations, e.g. in mutations of PKD1 or PKD2, which cause earlier or later onset of autosomal dominant polycystic kidney disease, respectively. iv) Subgroups of diseases may be classified for differential therapy, e.g. in mutations in NPHS2, which convey resistance to steroid treatment in nephrotic syndrome. v) Disease mechanisms can be studied in related monogenic animal models, e.g. in cystic kidney diseases, in which mouse models offered the first insights into disease mechanisms of renal cystic ciliopathies. vi) New drugs can be developed, for example by studying knockout animal models.
In Preclinical Models Genetic Kidney Disease Is Reversible
A hereditary illness called autosomal superior polycystic kidney disorder leads fluid-filled cysts to form on the kidneys, impairing their functioning. The kidneys acquire inflammatory and fibrosis, or damage, as a result of cyst formation. A mutation under one of two genotypes, PKD1 or PKD2, is the more common source of the condition, which could be handed down from parent to kid within households.
Also Check: Is Pomegranate Juice Good For Your Kidneys
Available Techniques For The Diagnosis Of Ikds
The availability of larger and more diverse reference datasets has shown that many previously reported pathogenic variants in fact have an allele frequency that exceeds the disease prevalence and can be reclassified as benign. As a general rule, clinicians should only act on variants that are classified as either pathogenic or likely pathogenic and should also consider reassessing old genetic results in the light of newly available data. It is evident that post-sequencing data analysis is becoming the key step in NGS. While the cost of sequencing has been declining rapidly, the amount of sequence data generated is expanding, as a consequence of which data analysis and storage are accounting for larger fractions of the real cost of sequencing .
Clinicians should be aware of the potential psychosocial implications that a genetic diagnosis has for patients. There is a need for a multidisciplinary approach to genetic testing for IKDs. It does not seem feasible that all nephrologists requesting a genetic test will be sufficiently proficient to interpret any kind of genetic report appropriately. For example, many nephrologists do not know about the very common finding of variant of unknown significance. A multidisciplinary team comprising molecular geneticists, nephrologists, psychologists and genetic counselors should help in delivering this kind of genetic result to patients.
Copy Number Variation And Larger Chromosomal Re
Copy number variants are genetic structural variants which involve DNA regions being deleted or duplicated. This can occur throughout the genome affecting stretches of DNA ranging from kilo- to mega-base pairs in length and can result in abnormal gene amplification . CNVs can be both inherited and arise de novo, and are increasingly being recognized as a significant source of genetic variation relating to both population diversity and disease, including renal diseases , neuropsychiatric diseases , and cancer .
There is often uncertainty about the genetic basis of CKD in pediatric patients, but recent studies have indicated that chromosomal microarrays have the potential to partly address this. Verbitsky et al. assessed 419 children enrolled in the CKD in children study alongside 21,575 children and adults who had undergone microarray genotyping for non-CKD studies. CNV disorders were identified in 31 children with CKD and 10 known pathogenic genomic disorders were detected including HNF1B deletion at 17q12. A further 12 pathogenic genomic imbalances were identified using this technique, distributed evenly among patients diagnosed with congenital and non-congenital forms of CKD. Overall, large gene-altering CNVs were more common in the CKiD population compared with the controls , but the specific genetic alterations identified in several of the individuals would require personalized recommendations in future healthcare.
Recommended Reading: Does Red Wine Cause Kidney Stones
Many Renal Tubular Disorders Allow Unequivocal Genetic Diagnostics
Renal tubular function governs reabsortion of water and solutes from the golmerular filtrate. An increasing number of tubulopathies are being recognized as caused by single-gene mutations . For some diseases, such as Bartter syndrome, similar disease phenotypes may be caused by mutations in different genes. The single-gene basis of renal tubulopathies allows for unequivocal molecular genetic diagnosis.
Identify Diagnosis Of Unknown Causes
While diabetic and hypertensive kidney diseases are the most common causes of kidney failure, there are others. There are instances when providers find themselves unable to identify the cause of kidney disease. Indeed, in some cases, urinalysis is actually bland and the workup to identify the cause of kidney disease is negative.
Even a kidney biopsy may not be helpful. It may show glomerulosclerosis and fibrosis . This does not help identify the original cause of kidney disease. Genetic testing can have a tremendous value in these cases. In fact, whole exome sequencing was able to diagnose up to one third of the patients who had unknown causes of kidney disease.
Recommended Reading: Kidney Pain Std
Evaluation Of Inherited Kidney Diseases
The Inherited Kidney Disease Clinic provides education, counseling and treatment, working with patients and families to navigate their available options for both genetic testing and clinical trials of experimental therapies. We collaborate closely with our patients’ referring physicians to coordinate treatment planning and follow-up care.
Some of the genetic conditions evaluated in the clinic include:
- Autosomal Dominant Polycystic Kidney Disease : The most common inherited kidney illness, ADPKD causes cysts to form on the kidneys. It occurs in about one in 800 people, and is passed down from parent to child through generations. Major health problems from ADPKD usually occur in adulthood, with more than 30,000 people in the U.S. each year suffering kidney failure as a result.
- Autosomal Recessive Polycystic Kidney Disease : This condition is also characterized by cysts, and affects about 1 in 20,000 people. ARPKD generally causes symptoms in early to late childhood. Learn more about dominant and recessive polycystic kidney disease on the PKD Foundation website.
- Thin Basement Membrane Disease
- Gitelman and Bartter Syndromes
- Collagen-related kidney diseases including Alport Syndrome: Learn more about Alport Syndrome on the Alport Syndrome Foundation website.
- Lowe Syndrome: Learn more about Lowe Syndrome on the Lowe Syndrome Association website.
- Hereditary Interstitial Kidney Disease: Gout associated inherited kidney diseases
- Tuberous Sclerosis
Apol1 Variants And Increased Likelihood Of Kidney Disease
The APOL1 risk variant does not seem to increase the risk of developing diabetic kidney disease, however it does appear to increase the risk of end-stage kidney disease in people with high blood pressure by 7 to 11 times.
APOL1 risk variants also increased the incidence of focal segmental glomerulosclerosis by 17 times, HIV-associated nephropathy by 29 to 89 times and nondiabetic kidney disease by 2 to 4 times, as well as increases in the development of other kidney diseases.
However, not all people with these genetic variations develop kidney disease. And people can still develop kidney disease without any genetic variant.
Read Also: Blood In Kidney Causes
So Why Do People With Certain Genetic Variants Develop Kidney Disease
We know that genetic variants are not solely responsible for the development of kidney disease. There are other factors that contribute to your kidney disease risk.
For many, the risk of developing kidney disease is not because of any one single reason, but due to a number of factors.
Environmental and social factors play a role in influencing and changing the way genes work. Some of the different types of factors include having more than one disease , where you live, work, and play.
While all these factors present challenges and obstacles to good health, there are also individual decisions and personal choices, which contribute to an increased risk of developing kidney disease. Some of these personal decisions include choosing to smoke, not being physically active or exercising, eating unhealthy foods, ignoring your mental health, and other individual behaviors and choices you make in your everyday life.
The illustration below shows how genetic variants, when combined with other factors, can increase your risk of developing several types of kidney diseases.
How Will I Know If I Have Adpkd
Children sometimes have symptoms of ADPKD, but people with the disease usually do not notice symptoms until they are between 30 and 50 years old. Symptoms might include:
If you have any of these symptoms, contact your health care provider. He or she may want to test for kidney problems. If your health care provider thinks ADPKD may be causing your symptoms, he or she may want you to have one or more of the following tests:
- Imaging tests, such as ultrasound, CT scans and MRI scans
- Genetic tests, using a sample of your blood or saliva
The imaging tests may be done to look for visible signs of cysts in your kidneys. The genetic tests can tell your doctor exactly what kind of PKD you have or if you are likely to develop the disease in the future. It can take months to get the results of genetic tests.
Read Also: Is Red Wine Good For Kidney Stones
Diagnosis Of Polycystic Kidney Disease
The severe symptoms of autosomal recessive PKD usually result in a prompt diagnosis. However, in most cases of autosomal dominant PKD, for many years there are no signs that a person has the condition.Physical check-ups or blood and urine tests may not always identify the disease. It is often detected during medical investigations for other health problems, such as urinary tract infections. At other times, the disease isn’t discovered until the kidneys begin to fail.
Diagnosis of PKD may involve a number of tests including:
- physical examination can detect symptoms such as high blood pressure or enlarged kidneys
- blood tests to assess kidney function
- urine tests blood or protein may be found in the urine
- ultrasound a simple, non-invasive test that can identify even quite small cysts
- genetic testing this is not a routine test but may be used for family testing. The presence of the abnormal genetic material can be detected with special blood tests. Genetic counselling is available for affected couples.
The Role Of Genetic Testing In Kidney Disease
Dr. Ali G. Gharavi
A new study at Columbia University Vagelos College of Physicians and Surgeon has found that genes cause about 1 in 10 cases of chronic kidney disease in adults, and that identifying the responsible genes has a direct impact on treatment for most of these patients.
Our study shows that genetic testing can be used to personalize the diagnosis and management of kidney disease, and that nephrologists should consider incorporating it into the diagnostic workup for these patients, says Ali G. Gharavi, MD, Chief of Nephrology at NewYork-Presbyterian/Columbia University Irving Medical Center, and a co-senior author of the study published in the January 10, 2019, issue of The New England Journal of Medicine.
It is estimated that 1 in 10 adults in the United States have chronic kidney disease. Yet, for 15 percent of patients with chronic kidney disease, the underlying cause of kidney failure is unknown. There are multiple genetic causes of chronic kidney disease, and treatment can vary depending on the cause, says Dr. Gharavi. And because kidney disease is often silent in the early stages, some patients arent diagnosed until their kidneys are close to failing, making it more difficult to find the underlying cause.
Most common diagnostic genetic findings: In total, 312 genetic diagnoses, representing 66 distinct monogenic disorders, were detected in 307 patients, with 5 patients harboring dual molecular diagnoses.
Don’t Miss: Is Watermelon Bad For Kidneys