Impact And Consequences Of Shpt: Bone Disease
Renal osteodystrophy refers to several bone disorders that accrue from thepathophysiology of bone and mineral metabolism in CKD: osteitis fibrosacystica, osteomalacia, and adynamic bone disease. Osteitis fibrosa cystica isreferred to as high-turnover bone disease and is associated with elevated PTHconcentrations that stimulate osteoclast activity, bone breakdown, andresorption. Osteomalacia is characterized by a lowturnover of bone and abnormal mineralization and has historically beenassociated with aluminumtoxicity.,Adynamic bone disease is referred to as low-turnover disease with normalmineralization and may result from low PTHlevels. Theprevalence of adynamic bone disease isincreasing andmay be the consequence of PTH over-suppression from the use of vitamin Dagents, calcimimetics, and phosphate binders, singly or in combination.
Kidneys Turning To Stone With Complete Kidney Failure
If Kidney stones are not bad enough, kidney failure is the next step and this can occur in people with hyperparathyroidism if the parathyroid tumor is not removed. In these cases the calcium collects within the kidney tissues instead of in the kidney tubes that make urine. So instead of getting stones, their entire kidney turns into stone! This is called “nephrocalcinosis“, meaning: nephro = kidney calcin = calcium osis = condition therefore “nephrocalcinosis” means “a condition by which the kidney tissues become full of calcium”. Said differently, their kidneys are so full of calcium that they are turning to bone! If a person has nephrocalcinosis, then we know that 1) they have had high blood calcium for over a decade, 2) their doctor has been asleep and ignoring high blood calcium. Nephrocalcinosis is almost always avoidable and is caused by doctors “watching” the patient’s high blood calcium for years saying “it isn’t that that high, we can watch it a while longer.”
Today we removed a huge, 15 year old parathyroid tumor out of Jane’s neck. The entire operation took 16 minutes and she went home just over 1 hour later. Her other three parathyroid glands were perfectly normal . I told Jane to expect her kidney failure to improve slowly, just a little bit, however it is possible that this parathyroid tumor was removed too late. It is possible that she will need a kidney transplant.
How Do Kidneys Keep Bones Healthy
Healthy kidneys also help keep your bones healthy. They do this in two ways:
- Your kidneys keep the right amounts of phosphorus and calcium in your body. When your kidneys are not working well, too much phosphorus can build up in your blood. This is called hyperphosphatemia.
- Your kidneys also help your body use vitamin D. When your kidneys are not working, your body may not be able to use vitamin D like it should. This can also cause your bones to get weak.
Too much phosphorus or not enough vitamin D in your blood puts you out of balance. Your body tries to “fix” this by making more of a hormone called parathyroid hormone . When your parathyroid makes too much PTH, its called secondary hyperparathyroidism. PTH pulls calcium from your bones to try and put your blood back in balance. This loss of calcium can eventually cause bone disease.
Recommended Reading: What Organ System Does The Kidney Belong To
Parathyroid Hormone Measurement In Chronic Kidney Disease: From Basics To Clinical Implications
Kittrawee Kritmetapak
1Division of Nephrology, Department of Medicine, Faculty of Medicine, Khon Kaen University, Khon Kaen 40002, Thailand
2Division of Endocrinology and Metabolism, Department of Medicine, Faculty of Medicine, Khon Kaen University, Khon Kaen 40002, Thailand
Abstract
1. Introduction
Chronic kidney disease-mineral and bone disorder , characterized by deranged metabolism of calcium, phosphate, parathyroid hormone , fibroblast growth factor 23 , and vitamin D bone abnormalities, formerly known as renal osteodystrophy and vascular calcification, is a well-established complication of CKD . CKD-MBD contributes to the large burden of cardiovascular disease, which is the leading cause of death in patients with CKD . The complex pathophysiology of CKD-MBD involves a number of feedback loops between the kidney, parathyroid glands, bone, intestine, and vasculature, and usually commences early in the course of CKD prior to the onset of clinically detectable abnormalities in serum calcium, phosphate, PTH, and vitamin D levels . Previous studies demonstrated that patients with CKD have decreased renal Klotho expression as early as CKD G1. As CKD progresses, Klotho concentration continues to decline, causing FGF23 resistance and, therefore, leading to marked increases in serum FGF23 and PTH levels , as well as decreases in serum 25-hydroxyvitamin D D) levels . However, hypocalcemia and hyperphosphatemia are usually observed in CKD G4G5.
4. Evolution of PTH Assays
Evaluation Of Active Vitamin D Therapy And Outcomes
Multiple observational studies have shown an association between the use of active vitamin D therapy in patients on dialysis and with CKD and improved survival. These range from larger studies from databases of dialysis providers to smaller cohort studies . Active vitamin D therapy has also been associated with slower progression to ESRD . There are a few studies in the literature in which an association between activated vitamin D use and improved survival was not found . One of these studies showed a mortality benefit for vitamin D using traditional models and marginal structural models but not when using a more complicated modeling system called instrumental variable models . The other study did show an association with improved all-cause mortality but not with specific causes of mortality such as cardiovascular or infection , suggesting the possibility that perhaps all of these specific causes are influenced by vitamin D and thereby diluting the effect on any individual one. There are no published reports of associations between nutritional vitamin D supplementation and improved survival in kidney disease, and data are mixed in the general population .
Don’t Miss: Carbonation And Kidney Stones
What Are The Causes
Where are the parathyroid glands?
We usually have four parathyroid glands in our neck, located just behind or within the thyroid gland, and they control the amount of calcium in our blood and bones. We need calcium in our blood for our nervous and muscular systems to function properly, and calcium in our bones to keep them strong.
Three things cause increased production of PTH: low blood calcium, low levels of activated vitamin D, and high phosphate levels. All three occur in chronic kidney disease.
How does kidney disease affect the glands?
Healthy kidneys activate Vitamin D so we can absorb calcium from our food. In advanced kidney disease the kidneys are unable to activate vitamin D so less calcium is absorbed and blood calcium levels fall.
This triggers the parathyroid glands to overproduce PTH in an attempt to increase the amount of calcium in the blood. PTH then increases calcium absorption from food, but also takes calcium out of the bones, creating high blood calcium levels. This can coincide with another bone mineral imbalance high levels of phosphorus in the blood . This happens when the damaged kidneys are unable to get rid of excess phosphate into the urine and it can cause itching and bone disease.
Secondary Hyperparathyroidism: Symptoms Causes & Treatment
Secondary hyperparathyroidism is common in people who have kidney failure . It happens when your bodys levels of calcium, vitamin D and phosphorus are not in balance. It is important to treat secondary hyperparathyroidism to prevent it from causing other health problems, such as bone disease.
Also Check: Can Seltzer Water Cause Kidney Stones
What Can Cause The Levels Of Pth Intact To Rise
The major cause of a rise in PTH Intact levels is kidney damage. An individual with impaired kidney function will not be able to balance the bodys electrolyte levels, especially phosphorus and calcium. Some drugs can cause an increase in Intact PTH levels, such as phosphates, steroids and anticonvulsants. Also, some heredity factors may play a role in a rise in PTH levels, such as familial hyperparathyroidism and MEN-I syndromes.
Skeletal Integrity Health And Bone Turnover Considerations
Abnormal skeletal structure and function are relatively common findings in patients with CKD . This is especially so in patients requiring dialysis . Extraskeletal soft tissue calcification is often a feature of CKD-MBD . It is likely that vitamin D has bimodal concentration-dependent propensities to retard or advance soft tissue calcium deposition . This important interplay between skeleton, vessels, and outcomes was recognized by the Kidney Disease Improving Global Outcomes initiative in its CKD-MBD position paper of 2006 .
The gold standard for diagnosis of the skeletal component of the CKD-MBD triad is biopsy-based histomorphometric analysis of bone biopsy specimens. However, bone biopsy, a painful and invasive procedure, is now much less commonly performed in clinical practice, and clinical and laboratory support for these procedures has waned substantially as a result. There are four significant bone diseases that we recognize as occurring in CKD: osteitis fibrosa cystica, low-turnover or adynamic bone disease, osteomalacia, and mixed uremic osteodystrophy . Hyperparathyroidism, due to progressive phosphate retention and lack of vitamin D activity, is the major promotor of the development of osteitis fibrosa. Near-universal sustained elevation of PTH concentrations is seen by the time dialysis therapy begins .
Studies comparing bone histomorphometry and plasma biomarkers of bone turnover in adults with CKD
Don’t Miss: Can A Kidney Infection Cause Diarrhea
What Does Early Kidney Disease Do To My Bones
As you read above, you need healthy kidneys to keep healthy bones. When you have kidney disease your bones are also at risk.
In the very early stages of CKD, you will probably not have any problems with how your body controls your phosphorus. However, if your kidney disease gets worse, you may also start to have problems controlling your phosphorus.
Talk to your doctor about what your phosphorus levels should be. Learn about the tests and symptoms of bone disease here
Are There Any Complications Of Hyperparathyroidism
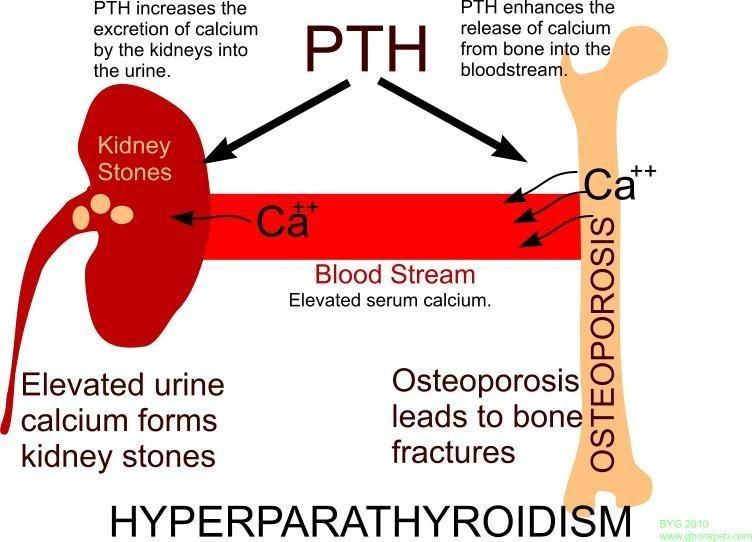
Not everyone with hyperparathyroidism has complications. However, sometimes complications may develop. If you have primary or tertiary hyperparathyroidism, these complications are mostly due to a long-standing high level of calcium in your blood. They can include:
- Kidney stones. Small stones may be passed in the urine without you noticing. Larger stones may get stuck, causing pain in your loin area that you then feel in your groin. You may also notice blood in your urine. See the separate leaflet called Kidney Stones for more details.
- Corneal calcification. Calcium can collect in the surface covering of your eye . This doesn’t usually cause any symptoms.
- Pancreatitis. This is inflammation of your pancreas gland. Rarely, a high level of calcium due to hyperparathyroidism can cause pancreatitis. This can cause severe upper tummy pain. See the separate leaflet called Acute Pancreatitis for more details.
- Stomach ulceration. A high calcium level can make your stomach produce too much acid and lead to stomach ulceration. See the separate leaflet called Stomach Ulcer for more details.
- Kidney damage. A prolonged high calcium level in your blood can damage your kidneys and cause CKD.
Also Check: Can You Have 4 Kidneys
How Do I Prevent Bone Disease
If you have kidney disease, it is important to manage your phosphorus levels. This can help prevent bone disease.
Steps you can take to manage your phosphorus levels include:
- Take a phosphate binder
- This is a pill you take with meals
- Keeps your body from absorbing the phosphorus from foods and drinks
- Help keep phosphorus from building up in your blood.
What Happens To Pth When The Kidney Fails
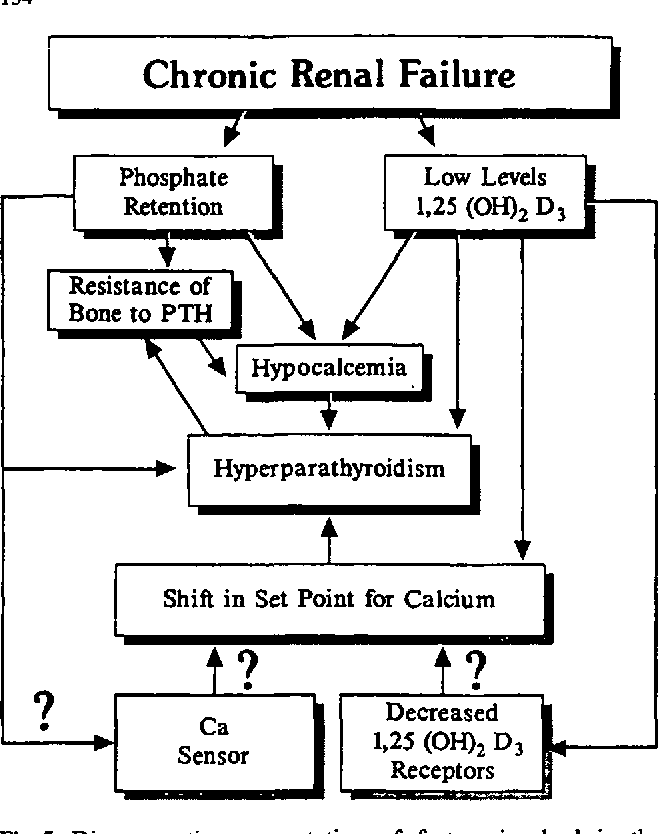
There are several reasons why an increase in PTH is common with kidney failure. This happens about three times more common in women than men and patients are usually older, with an average age at presentation of 65 years , according to The American Association of Endocrine Surgeons.
As blood phosphorus levels rise, so do PTH levels. With the PTH levels risen, the diseased kidney cannot activate vitamin D. Without activated vitamin D, calcium cannot be absorbed from your intestines into your blood. When the blood calcium level drops, the parathyroids respond by producing more PTH. This is when hyperparathyroidism often develops. Hyperparathyroidism is the enlargement of the parathyroid glands. Then, more PTH is produced to counter-attack the low blood calcium level.
Recommended Reading: Is Honey Good For Kidney
What Does Kidney Failure Do To My Bones
As kidney disease gets worse, so do many other problems. When your kidneys fail and you need dialysis or a transplant, you will need to be very careful in how you manage your phosphorus. The good news is, there are many ways to manage your phosphorus through medicine and diet.
Talk to your healthcare team about how to best manage your phosphorus so that you prevent bone disease. How you manage your phosphorus will depend on several things, including:
- Your usual diet
- The kind of dialysis you are doing
- The medicines you are taking
- How your lab numbers are doing
If you are on dialysis, it is very important that you do not skip dialysis treatments! Your doctor may also suggest changing the number and length of dialysis sessions to get rid of extra phosphorus.
Can The Parathyroid Cause Kidney Failure
by Jessica | Apr 29, 2020 | Parathyroid
Hyperparathyroidism is a condition that causes one or more parathyroid glands to produce an excess amount of parathyroid hormone . This disrupts the blood calcium level in the body and can lead to kidney failure. To understand the correlation between parathyroid gland abnormalities and kidney failure, lets examine the impact of HPT on the kidneys.
You May Like: Is Honey Good For The Kidneys
What Can I Do To Keep My Serum Calcium Level Normal
Eat a well-balanced diet. Other nutrients such as magnesium and vitamin D are needed to absorb calcium. A dietitian who works with kidney patients can help you plan a diet that fits your individual needs. Dairy foods are high in calcium, but may also be high in phosphorus, which is usually limited in CKD. Your dietitian can help you find healthy alternatives to many high phosphorus foods.
You may need a vitamin D supplement, but your healthcare team will need to order the right one for you. Dont take a vitamin D supplement or a calcium supplement unless your healthcare team orders one for you. If you need a medicine called a phosphate binder to lower your phosphorus, then your healthcare team may recommend one that has calcium.
Bone Metabolic Markers In Ckd Patients
Bone markers reflect the activities of bone cells. They are divided into two subgroups humoral factors derived from bone cells, and factors associated with type-I collagen metabolism. Of the bone cell-derived factors, those secreted by osteoclasts are regarded as bone resorption markers, and those originating from osteoblasts are regarded as bone formation markers, except for under-carboxylated osteocalcin, which also reflects vitamin K status.
Bone remodelling is the lifelong process by which mature bone is removed and new bone is formed it is also the mechanism allowing skeletal growth, bone reshaping and the replacement of injured bone following fractures and micro-damages. Bone remodelling is also crucial for the regulation of circulating calcium and phosphate levels. Dialysis patients display extremely high risk of hip fracture . Nevertheless, modern clinical studies repeatedly demonstrated that PTH levels show only a limited association with hip fracture risk .
Also Check: Can Seltzer Water Cause Kidney Stones
Measurement Of Pth In Real Life: Its Just Not As Simple As Checking A Box Or Pressing A Button
In requesting and interpreting laboratory investigations, we must always ask the questions: What is the result of this test going to do for the betterment of the patients health, and is the test itself reliable as a marker of illness or outcomes? The dangers of believing that test result numbers equate to illness or health, or that an automatic response to normalize these numbers is appropriate, have now been masterfully spelled out in relation to both anemia and CKD-MBD . If there is no obvious utility, there is futility.
However, for PTH we must also understand important inherent potential biases and inaccuracies relating to numerous analytic and preanalytic factors.
Why Do Kidney Disease Patients Have High Calcium Level
Kidney disease patients are at the risk of both high calcium level and low calcium level, but low calcium level is more common than high calcium level. Thereby, we are here to introduce more about high caclium level for kidney patients.
The causes of high calcium level in CKD
To monitor the progression of chronic kidney disease, patients are often suggested to do blood test and urine test. If their calcium level is higher than 2.75 mmol/L, it indicates their calcium level is higher than the normal. Generally, the following conditions can cause the elevation of high calcium level.
1. Extra intake of vitamin D, vitamin A or other metabolic products. These substances can prompt the calcium absorption in intestinal tract. Then, calcium level in the blood increases gradually.
2. The use of thiazide diuretics. These medicines can stimulate more fluid to eliminate out of the body, resulting in low blood volume and increasing the calcium reabsorption by renal tubules. The decline of calcium excretion can trigger high calcium level.
3. Kidney Failure: In the oliguria stage of acute kidney failure, calcium cant be excreted by urine but accumulates in the soft tissues. In this condition, hypocalcemia can cause the increase of PTH, so as to increase the absorption of calclium by bone. Finally, hypercalcemia occurs easily.
How to lower high calcium level for kidney patients?
Recommended Reading: Seltzer Water And Kidney Stones