First Successful Transplant Of A Pig Kidney Into A Human Performed
The first successful transplant of a pig kidney into a human was performed on Saturday, September 25, 2021, at the New York Universitys Langone Transplant Institute.
The kidney was obtained from a pig that had undergone gene editing to knock out a sugar molecule that elicits a devastating immune response in humans and has been responsible for the failure of previous attempts at cross-species transplantation, so called xenotransplantation, said lead investigator Dr. Robert Montgomery who led a surgical team in a two-hour operation. Biopsies taken every 12 hours and viewed under the microscope showed no evidence of rejection.
The transplant was performed on a patient who was already brain dead. According to a press release by NYUs Lagone Transplant Institute the family graciously approved donation of their loved ones body for this procedure.
The kidney was obtained from a genetically engineered pig hundreds of miles away and transplanted into a deceased donor. The donor was maintained on a ventilator, with the consent of the family, for 54 hours while doctors studied the kidneys function and watched for signs of rejection, said NYU.
What was profound about these findings is that the pig kidney functions just like a human kidney transplant, said Dr. Mongomery. Individuals who receive a kidney transplant on average live twice as long and with a better quality of life as patients who remain on dialysis. However, human organs for transplantation are scarce.
First Living Donor Hiv
Donor Nina Martinez with transplant surgeon Dorry SegevCredit: Johns Hopkins Medicine
Correction: The information in this news release has been updated as of April 11 to reflect a correction to previously reported information. On March 25, 2019, Johns Hopkins Medicine performed the first living donor HIV-to-HIV kidney transplant in the United States. It was previously reported as the first in the world.For the first time in the U.S., a person living with HIV has donated a kidney to a transplant recipient also living with HIV. A multidisciplinary team from Johns Hopkins Medicine completed the living donor HIV-to-HIV kidney transplant on March 25. The doctors say both the donor and the recipient are doing well.
This is the first time someone living with HIV has been allowed to donate a kidney, ever, in the nation, and thats huge, says Dorry Segev, M.D., Ph.D., professor of surgery at the Johns Hopkins University School of Medicine. A disease that was a death sentence in the 1980s has become one so well-controlled that those living with HIV can now save lives with kidney donationthats incredible.
Dont call me a hero, call me the first. I want to see who comes next.
In July 2018, Martinez read on Facebook that a friend who also happened to have HIV needed a kidney transplant. Martinez felt compelled to look for a way to bring HOPE to her friend. Familiar with the medical research process and public health policy, she contacted Johns Hopkins.
Success In Organ Transplantation
At only 23 years old, Richard Herrick was dying. After his discharge from the Coast Guard, Richard went home to Massachusetts to be with his family when he was diagnosed with kidney disease. At the time, this diagnosis was a death sentence and by October of 1954 his health was deteriorating. Most transplant donors at this time were biological relatives of the recipient to reduce the risk of organ rejection. Luckily, Richard had an identical twin brother, Ronald.
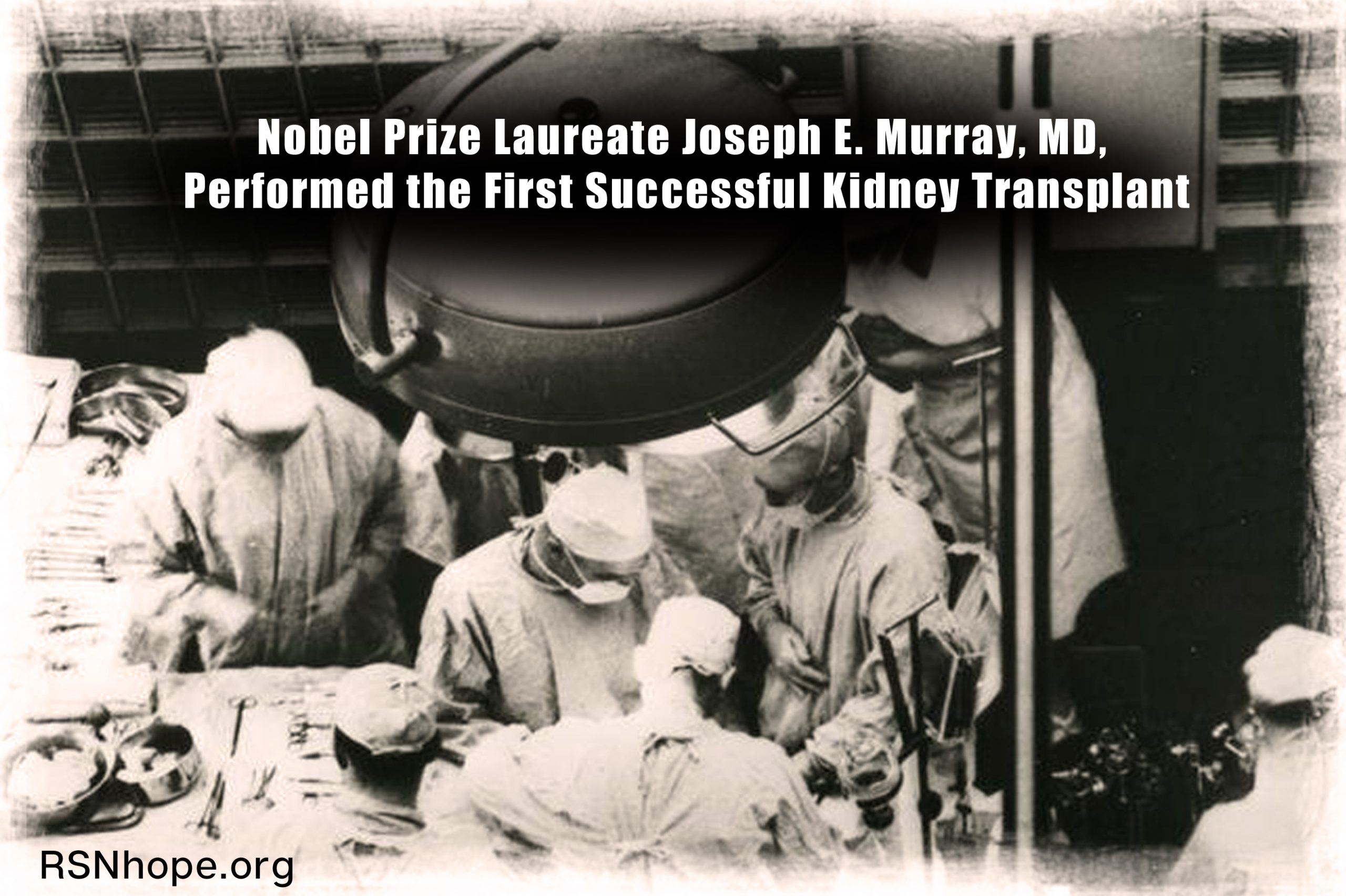
A team of local doctors at Bostons Peter Bent Brigham Hospital had already successfully completed a series of human kidney grafts, some of which functioned for days or even months, they were willing to attempt the transplant between Richard and Ronald. In December of 1954 the surgeons, led by Dr. Joseph E. Murray transplanted a kidney from Ronald into his twin brother Richard since donor and recipient were genetically identical, the kidney was not rejected, and the procedure was a success.
Also Check: Carbonated Water Kidney Stones
In The Us Health System
Transplant recipients must take immunosuppressive anti-rejection drugs for as long as the transplanted kidney functions. The routine immunosuppressives are tacrolimus , mycophenolate , and prednisolone these drugs cost US$1,500 per month. In 1999 the United States Congress passed a law that restricts Medicare from paying for more than three years for these drugs unless the patient is otherwise Medicare-eligible. Transplant programs may not transplant a patient unless the patient has a reasonable plan to pay for medication after Medicare coverage expires however, patients are almost never turned down for financial reasons alone. Half of end-stage renal disease patients only have Medicare coverage. This provision was repealed in December 2020 the repeal will come into effect on January 1st 2023. People who were on Medicare, or who had applied for Medicare at the time of their procedure, will have lifetime coverage of post-transplant drugs.
The United Network for Organ Sharing, which oversees the organ transplants in the United States, allows transplant candidates to register at two or more transplant centers, a practice known as ‘multiple listing’. The practice has been shown to be effective in mitigating the dramatic geographic disparity in the waiting time for organ transplants, particularly for patients residing in high-demand regions such as Boston. The practice of multiple-listing has also been endorsed by medical practitioners.
A Period Of Consolidation
The next quarter century, 19641980, is often classified as a period of consolidation or plateau. During this period, except for the development of antilymphocytic serum , there were no landmarks. Importantly, however, there was steady progress. Practical innovations and accomplishments took place that were necessary for maturation of kidney transplantation into a useful clinical service. These included availability of dialysis Medicare funding of end-stage renal disease antibody screening to avoid hyperacute rejection the importance of tissue typing for related donor transplants acceptance of brain death ex vivo preservation, allowing donor organs to be transported and shared , and, perhaps most importantly, the accumulation of experience in patient management that led to the avoidance of over-immunosuppression, thereby decreasing resultant infections and deaths.
Don’t Miss: Is Wine Bad For Kidney Stones
The Life Of Yuri Vorony
Yuri Yurijevich Voronoy was born in 1896 in the village of Zhuravka in Poltava , where his father was a professor of mathematics . After receiving a medical education in Kiev and graduating in 1921, Voronoy spent his life working as a surgeon and researcher, either in Kiev or in the nearby major cities in the Ukraine. His formative years seem to have been from 1926 to 1931, when he was a member of the Department of Surgery at Kharkov, headed at that time by Professor Shamov. One of the departments interests was in blood transfusion and they pioneered the Soviet method of using cadaveric blood for this purpose. Another interest of the department at that time was testicular transplantation in man. The reason for this odd and doubtful project was that the Russian surgeon Serge Voronoff , was touring Europe and the world in the late 1920s and claiming plausibly that the transplantation of the testis from monkeys to jaded or ageing humans would rejuvenate and revive them . Thus, Voronoy began work to in a department interested at that time in blood transfusion and testicular transplantation.
Figure 3
The first publication of the first human kidney transplantation in Spanish journal El Siglo Medico .
/7 Assistance To Place Organs
In 1982, SEOPF establishes the Kidney Center, the predecessor of the UNOS Organ Center, for round-the-clock assistance in placing donated organs.
1981
1983
First successful single-lung transplant performed.
Cyclosporine, the first of a number of drugs that effectively treat organ rejection by suppressing the human immune system, introduced.
Also Check: Is Ginger Tea Good For Kidneys
Review Of The Literature In Soviet Union To First Kidney Transplantation
The publications of Mirski und Korol et al. uncover several imprecise elements of Voronoys biography . Particularly, the date of the performed kidney transplantation was claimed as 1930 by some authors, which is incorrect . This date represents the time of the third Congress for physiologists where Voronoy presented his experimental work in the dog. Furthermore, Korol et al. pointed out the fact that the first human kidney transplantation was not performed by Voronoy in the year 1934 in Paris, but in 1933 in Kherson . These corrections are based on Voronoys original work, which was published in a Spanish journal in 1936, and in 1934 in the Russian language .
Statement About Operation And Autopsy
How can the described changes in the allograft kidney be described? Obviously, in the first line stands the toxic effect of the mercury. Furthermore, the postoperative blood transfusion seems to have had a toxic effect because the relatively high mercury concentration in the blood might have had a haemolytic effect on the transfused erythrocytes. These changes and particularly the consequence of a haemolysis could be seen in the postmortal preparation obviously. Also, the partially incompatible constellation of the blood type between the donor and the recipient should not be ignored, although the macro haematuria which did not occur simultaneously, but in a time interval after the transplantation, speaks against this point. It is obvious that even a short survival of the patient in our case 2days after kidney transplantation does not compromise this operation for this indication in any way. The clinical consequence from this case is that the performed blood letting therapy has to be accompanied by an infusion therapy and not by a blood transfusion therapy. In the case of a nonheart beating donor kidney transplantation, the technique, indication and contra-indication as well as the immunological mechanisms of the rejection should be overworked in detail.
You May Like: Is Cranberry Juice Good For Your Liver And Kidneys
National Research Council Conference
In 1963, one of the most important landmarks in the history of transplantation was revealed during a small conference organized by the National Research Council . About 25 individuals including most of the worlds active transplant clinicians and scientists assembled in Washington to review the status of human kidney transplantation. The results presented by these acknowledged experts were extremely discouraging. Less than 10% of their several hundred allograft recipients had survived as long as 3 months . Of patients treated with total body irradiation, only six had approached or achieved 1 year survival . Hope was expressed that immunosuppressive drugs might be more effective. Murray reported his first 10 patients treated with 6-MP and azathioprine instead of irradiation . One had survived for a year, although at the time of the conference it was failing. The others died within 6 months. Thus, at this point, drugs seemed no more effective than radiation. The mood at the conference was so gloomy that some participants questioned whether continued activity in human transplantation could be justified .
Also Read: Irresponsible Use Of Chemicals Drugs In Food Items Cause Of Kidney Diseases Cancer Nafdac
He added: After all the screenings, the third prospect was found to be fit. We were all happy and convinced that we were getting a solution to the problem. It was then the series of counselling session for both of us, the donor and recipient, began. We were severally counselled.
According to Dr. Stephen Olawale Oguntola, the Coordinator of the Transplant Programme and Lead Nephrologist with the ABUAD Multi-System Hospital, the transplant was done simultaneously on Wednesday, October 13, using a dedicated twin-transplant theatre right here in this Hospital, thus making it the first successful kidney transplant in Ekiti/Ondo axis of the country.
Oguntola added: the kidney function started improving right inside the theatre with the new kidney producing 2.3 litres of urine before the end of surgery which lasted for 5 hours, 15 minutes.
Thereafter, the kidney function has continued to make a sustained improvement. We are very happy about the way both the donor and recipient have responded to the procedure. Both of them are in very high spirits. In fact, the donor was discharged on October 20 and with the look of things, the recipient will be discharged in a couple of days to start his normal life after the transplant.
The Consultant Nephrologist thereafter called on members of the public to avail themselves of the facilities and equipment available in ABUAD Multi-System Hospital, stressing that ABUAD is an enclave of endless possibilities
You May Like: What Std Messes With Your Kidneys
Unmodified Animal And Human Kidney Transplants
In 1933, the Soviet surgeon Yu Yu Voronoy performed the first human-to-human kidney transplant. That the kidney was not procured until 6 hours after the donors death and that it was transplanted across a major blood group mismatch probably accounted for its prompt failure . Four other human homografts that Voronoy performed between 1933 and 1949 also failed rapidly. Published in Russian, this experience remained unknown in the West until the 1950s.
In the 1940s and early 1950s, experimental dog kidney transplantation was actively conducted by surgeons in Paris and Boston and also by Morton Simonsen in Denmark and William Dempster in London. The second set phenomenon was again observed, but no new insights emerged. Simonsen searched in vain for an antibody response, being unaware of Loebs work on the lymphocyte . Dempster, who joined Medawar in denouncing Loeb and his cellular theory of immunity, may have been the first to use radiation in organ transplant recipients . He also treated dog homograft recipients with cortisone , which Rupert Billingham had found to prolong survival of skin homografts in rodents . In dogs, neither treatment had much effect on rejection. Dempster like others despaired of further progress in organ transplants and advised against any attempt in humans.
Transplantation Research Of A Lost Era
Although consensus on the fate of homografts would not be reached for another 50 years, during the first decades of the twentieth century several well-known investigators established not only the inevitability of homograft failure but most of the other basic principles of transplantation immunology. In 1903, Paul Ehrlich studied transplantation of tumors in mice without bothering to determine the response to transplants of normal tissue . The use of tumor homografts confused the issue because they would sometimes overwhelm their recipients before being rejected. In the same year, the Danish biologist Carl Jensen perceived that the failure of tumor homografts was an immune reaction, but this explanation was discounted by Ehrlich because no antibody could be detected.
Georg Schöne may deserve recognition as the first transplantation immunologist. Working in Ehrlichs laboratory in 1912, he studied grafts of skin rather than tumors. He determined that homografts always failed and that subsequent grafts from the same donor failed more rapidly than the first . Three decades later, several surgeons would be squabbling for the credit of discovering this second set response, suggesting that they deserved a share of Medawars Nobel Prize, which in part was based on this landmark observation.
Read Also: Does Pellegrino Cause Kidney Stones
The First Organ Transplant
On June 17, 1950, Dr. Richard Lawler, Dr. James West and Dr. Raymond Murphy performed the first successful kidney transplant at Little Company of Mary Hospital, Evergreen Park, IL.
The patient, Ruth Tucker, was a 49-year-old with polycystic kidney disease . Both of Ruths kidneys had been damaged by PKD, one functioned at only 10% and the other no longer functioned. Ruths mother and sister had both died from PKD and because dialysis was not yet widely available, Ruth knew a kidney transplant was her only option to survive.
Tissue typing did not exist at this time, so organ selection for transplants was based on very basic criteria such as gender, blood type, and finding a donor roughly the same age and physical size as the recipient. A suitable match was found for Ruth after 5 weeks of waiting in the hospital her donor had died of cirrhosis of the liver. In an interview after the surgery, Dr. Lawler, commented: Not the most ideal patient, but the best we could find.
Dr. Lawler had performed a few experimental organ transplants in dogs and translated the knowledge he gained to perform Ruths transplant surgery. With roughly 40 other physicians looking on, Dr. Lawler and his team completed the procedure within 45 minutes after removal of the donor kidney. Ruth was released from the hospital 30 days later.
‘pig Kidney’ To People First Successful Xenograft Transplantation
2021-10-22T12:23:15.267Z
A US research team has succeeded in transplanting pig kidneys into humans. Research on transplanting animal organs into humans has been around for a long time, but this is the first time that an actual transplant has been successful.
< Anchor> An
American research team has succeeded in transplanting pig kidneys into humans. Research on transplanting animal organs into humans has been around for a long time, but this is the first time that an actual transplant has been successful.
Correspondent Kim Jong-won of New York.
< Reporter>
Pigs have organs that are most similar to humans, and research on organ transplantation between humans and pigs has been ongoing for a long time.
However, it was not successful because of immune rejection from transplantation of organs from other species, so-called xenogeneic livers.
Recently, however, a research team at New York University in the United States succeeded for the first time in transplanting a pig kidney into a patient who was brain-dead due to renal failure.
This transplantation was carried out with the pig kidney connected to the thigh, not the inside of the human body. It has succeeded in creating and performing normal kidney function.
In this experiment, pigs whose genes were edited so as not to cause immune rejection were used.
Recommended Reading: Is Mio Bad For Your Kidneys
On The 67th Anniversary Of The First Successful Kidney Transplant Here Are A Few Facts That You Would Not Like To Miss:
- Dr. Richard Lawler performed the world’s first kidney transplant
- Before performing the procedure on a human, Lawler had done few experimental organ transplants on dogs
- The recipient of the kidney transplant was an ailing 49-year-old Chicago woman, Ruth Tucker, who died after five years of the transplant
- It has been reported that the transplant took him only an hour and a half
- 40 other doctors watched the surgery
- The photographer, who filmed the transplant, fainted while filming, and it is said that one of the doctors had to take over the procedure of filming
- Dr Richard Lawler never performed another transplant because he did not want to be a transplant surgeon
- After the transplant, Lawler received many letters from other doctors wanting to learn the procedure from him and from patients seeking his services following the transplant surgery
- “I just wanted to get it started” was what Dr. Lawler said after being asked why he never performed another one.
Interested in General Knowledge and Current Affairs? to stay informed and know what is happening around the world with our G.K. and Current Affairs section.